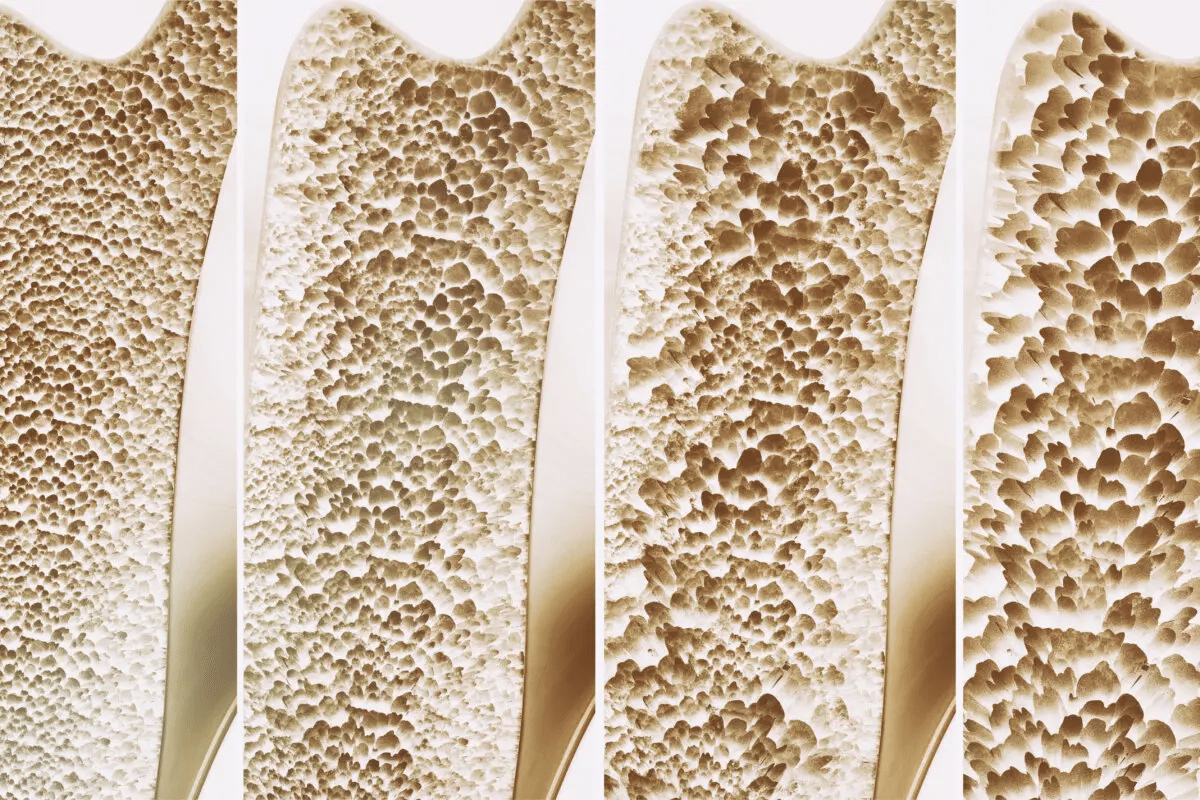
Bisphosphonates have been a key part of treating osteoporosis for over 20 years. They are used by both men and women. These drugs help stop bone loss by slowing down bone breakdown, which boosts bone density.Know the contraindications for bisphosphonates. This essential guide explains 5 key risks for osteoporosis patients taking these drugs.
It’s important to know the risks of bisphosphonate therapy. Some patients face big risks if these drugs are given without checking first. It’s key to look at who should not take them to keep treatment safe and effective.
Key Takeaways
- Bisphosphonates are a widely prescribed class of medications for treating osteoporosis.
- Understanding contraindications is critical for safe and effective treatment.
- Careful patient evaluation is necessary before prescribing bisphosphonates.
- Bisphosphonates work by inhibiting bone resorption to improve bone mineral density.
- Assessing patient risks is essential for successful osteoporosis management.
Bisphosphonates in Osteoporosis Treatment
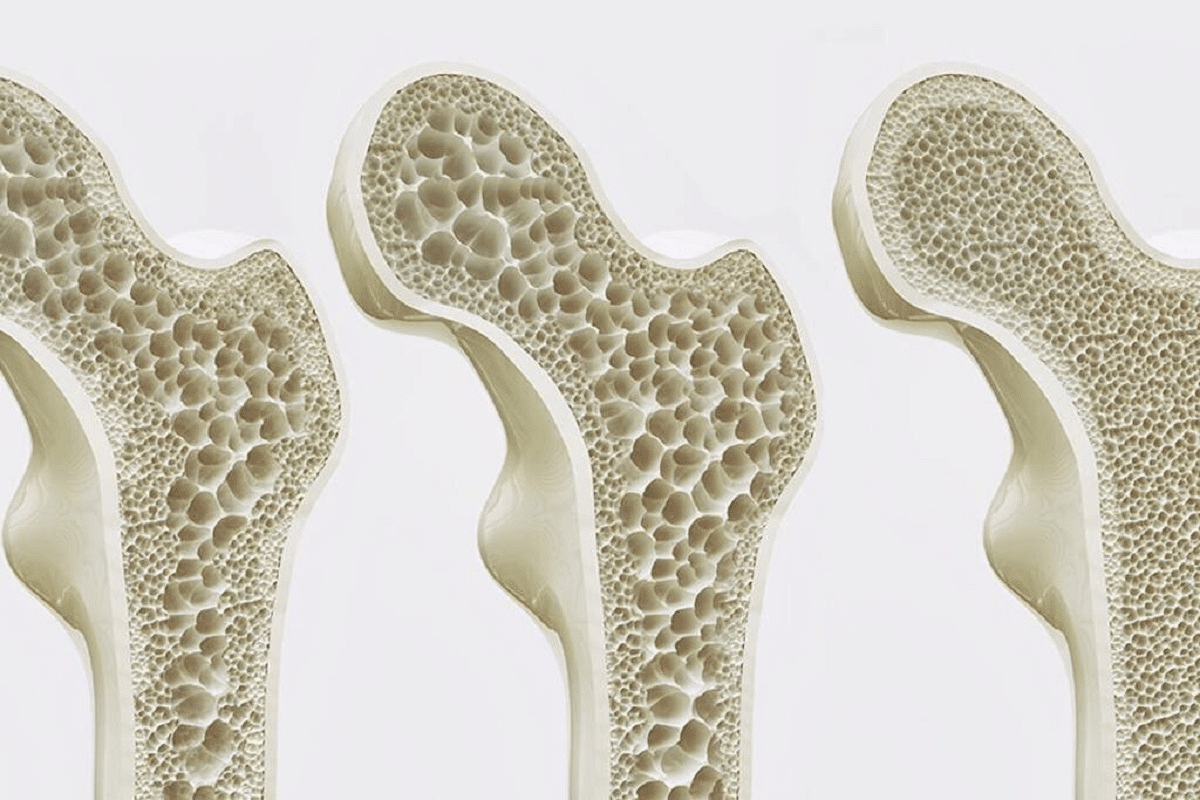
For over two decades, bisphosphonates have been key in fighting osteoporosis. They work by stopping bone breakdown. We’ll look at how these drugs have changed and the options they offer for treating osteoporosis.
Evolution of Bisphosphonate Therapy
Big strides have been made in bisphosphonate therapy. What started as a few options has grown to include many oral and intravenous forms. Alendronate, risedronate, ibandronate, pamidronate, and zoledronic acid are some of the bisphosphonates available today, making treatment more flexible.
These drugs have also gotten stronger and easier to use. The creation of nitrogen-containing bisphosphonates has made them even more effective. This class of bisphosphonates is now a key part of managing osteoporosis, helping to lower the risk of fractures.
Types of Nitrogen-containing Bisphosphonates
Nitrogen-containing bisphosphonates are a vital part of bisphosphonate drugs. Their unique structure makes them very good at stopping bone loss.
The most used nitrogen-containing bisphosphonates are alendronate, risedronate, and zoledronic acid. Studies have shown they can greatly reduce fracture risk in people with osteoporosis. They come in different forms, like pills and shots, to fit what each patient needs.
It’s important for doctors to know about the different nitrogen-containing bisphosphonates. This knowledge helps them choose the best treatment for each patient. By picking the right bisphosphonate, doctors can help patients live better lives.
Mechanism of Action of Bisphosphonates
It’s important to know how bisphosphonates work to understand their role in treating osteoporosis. These medications target the bone resorption process. This is key in managing osteoporosis.
Inhibition of Bone Resorption Process
Bisphosphonates mainly work by stopping bone breakdown. Osteoclasts are the bone cells that break down bone. By stopping them, bisphosphonates help keep bone density up.
They do this by binding to bone crystals. This action stops bone breakdown. It’s how bisphosphonates stay in the bone and work on osteoclasts.
Molecular Basis of Bisphosphonate Activity
At a molecular level, bisphosphonates block the mevalonate pathway. This pathway is key for osteoclasts. Bisphosphonates bind to bone, stopping the prenylation of proteins needed for osteoclasts to work and live.
The table below summarizes the key aspects of bisphosphonate mechanism of action:
|
Mechanism |
Description |
Effect on Bone |
|---|---|---|
|
Inhibition of Osteoclast Activity |
Bisphosphonates bind to hydroxyapatite, inhibiting osteoclast function |
Reduced bone resorption |
|
Molecular Inhibition |
Inhibition of the mevalonate pathway, preventing prenylation of GTP-binding proteins |
Impaired osteoclast activity and survival |
|
Clinical Outcome |
Maintenance of bone density, reduction in fracture risk |
Improved bone health |
In conclusion, bisphosphonates work by stopping bone breakdown and affecting osteoclasts at a molecular level. Knowing this helps us see why they’re good for osteoporosis treatment.
Clinical Benefits in Osteoporosis Management
Bisphosphonates are key in treating osteoporosis. They bring many benefits to patients. Let’s look at how these drugs help manage osteoporosis.
Improvements in Bone Mineral Density
Bisphosphonates boost bone mineral density (BMD). This is vital for lowering fracture risk. Studies show they can increase BMD by 5 to 7 percent in the spine and 1.6 to 5 percent in the femoral neck after three years.
This BMD increase is key for osteoporosis patients. It means a lower risk of fractures in the spine and other parts of the body.
Fracture Risk Reduction Timeline
The time it takes for bisphosphonates to lower fracture risk is important. Research shows they can cut fracture risk by up to 50 percent in the first year. Long-term use keeps this risk reduction going.
It’s important for patients and doctors to talk about bisphosphonate therapy. This helps make informed choices about managing osteoporosis.
Contraindications for Bisphosphonates: Hypocalcemia
Hypocalcemia is a big no-no for bisphosphonate treatment. We need to think carefully before starting it. This is to keep patients safe and make sure the treatment works well.
Pathophysiology of Hypocalcemia Risk
Hypocalcemia, or low blood calcium, can cause big problems with bisphosphonates. Bisphosphonates can make calcium levels even lower. This is bad news for people with hypocalcemia.
The pathophysiology involves the inhibition of osteoclast-mediated bone resorption. This is good for treating osteoporosis. But, it can make hypocalcemia worse if calcium levels are not right.
Things that raise the risk of hypocalcemia include vitamin D deficiency, kidney problems, and issues with the parathyroid gland. We need to spot these risks before starting treatment.
Pre-treatment Assessment Requirements
We do a detailed check before starting bisphosphonates. This is to find out who might get hypocalcemia. The check includes:
- Checking blood calcium levels
- Looking at vitamin D levels
- Checking how well the kidneys are working
- Looking at the patient’s medical history for signs of hypocalcemia
It’s very important to fix hypocalcemia before starting bisphosphonates. This might mean treating vitamin D deficiency or making sure calcium levels are normal.
Monitoring Guidelines During Therapy
After starting bisphosphonates, we keep a close eye on patients for hypocalcemia. The monitoring includes:
- Regular blood tests for calcium
- Watching for symptoms like muscle cramps or numbness
- Changing calcium and vitamin D supplements if needed
By watching patients closely and managing hypocalcemia well, we can lower the risks of bisphosphonate treatment. This helps our patients get the best results.
Severe Renal Impairment as a Critical Contraindication
Severe kidney problems make bisphosphonates a bad choice for treating osteoporosis. These drugs mainly leave the body through the kidneys. If a patient’s kidneys are very weak, the drug can build up and harm the kidneys more.
Before starting bisphosphonates, it’s important to check how well the kidneys are working. We look at the glomerular filtration rate (GFR) to do this.
GFR Thresholds for Different Bisphosphonates
Each bisphosphonate has its own GFR limit. If the GFR is below this limit, the drug should not be used or should be used with great care. Here are the GFR limits for different bisphosphonates:
|
Bisphosphonate |
GFR Threshold (mL/min) |
|---|---|
|
Alendronate |
35-45 |
|
Risedronate |
30 |
|
Ibandronate (oral) |
30 |
|
Ibandronate (IV) |
30 |
|
Zoledronic acid |
35 (or 30 in some guidelines) |
Mechanisms of Renal Toxicity
Bisphosphonates can harm the kidneys in several ways. They can damage kidney cells and even cause sudden kidney failure. The exact reasons are not fully known but might include:
- Direct harm to kidney cells
- Changes in how blood flows through the kidneys
- Formation of crystals in kidney tubules
Alternative Osteoporosis Treatments for Renal Patients
For those with severe kidney problems, other treatments for osteoporosis are needed. These include:
- Denosumab: A drug that stops bone loss without needing to adjust the dose for kidney problems.
- Teriparatide: A hormone that helps build bone and is safe for those with kidney issues.
- Raloxifene: A drug that can be used carefully in patients with kidney problems.
When treating osteoporosis in patients with severe kidney problems, we must think carefully about the risks and benefits. It’s important to watch the kidneys closely and adjust treatment plans as needed.
Upper Gastrointestinal Disorders and Esophageal Abnormalities
Upper gastrointestinal disorders and esophageal abnormalities are big no-nos for oral bisphosphonates in osteoporosis treatment. These drugs can irritate the esophagus. They’re not good for people with certain esophageal problems.
Specific Conditions Precluding Oral Bisphosphonate Use
Some upper gastrointestinal disorders and esophageal issues mean you can’t take oral bisphosphonates. These include:
- Esophageal strictures
- Achalsia
- Active esophagitis
- Barrett’s esophagus with dysplasia
People with these problems are more likely to hurt their esophagus with oral bisphosphonates. Doctors need to check a patient’s stomach and esophagus history before giving these drugs.
Pathophysiology of Esophageal Injury
Oral bisphosphonates can harm the esophagus in a few ways:
- Direct mucosal irritation
- Delayed esophageal transit
- Inadequate mucosal defense
This damage comes from cytokines and other inflammatory stuff. It can lead to serious esophagitis.
Intravenous Options for High-Risk Patients
For those with stomach or esophageal issues, intravenous bisphosphonates are a good choice. These include:
|
Medication |
Dosing Frequency |
Key Benefits |
|---|---|---|
|
Zoledronic acid |
Annual |
High adherence, effective fracture reduction |
|
Ibandronate |
Quarterly |
Less frequent dosing, reduced gastrointestinal side effects |
Intravenous bisphosphonates skip the stomach and esophagus. This makes them safer for those at high risk.
Practical Contraindication: Inability to Maintain Upright Posture
Bisphosphonates are key in treating osteoporosis. They help lower the risk of fractures. But, taking them right requires staying upright for a while.
Patients must stay upright for 30 to 60 minutes after taking oral bisphosphonates. This helps avoid esophageal irritation and other stomach problems.
The 30-60 Minute Post-dose Requirement
Staying upright for 30 to 60 minutes is important. It lets the medicine move safely through the esophagus and into the stomach. The exact time needed can change based on the medicine and the patient’s health.
Here’s a table showing how long to stay upright after taking different bisphosphonates:
|
Bisphosphonate |
Post-dose Upright Time |
|---|---|
|
Alendronate |
30 minutes |
|
Risedronate |
30 minutes |
|
Ibandronate |
60 minutes |
Consequences of Improper Administration
Not staying upright after taking oral bisphosphonates can cause serious problems. These include esophagitis, ulcers, and even stricture or perforation. These risks are higher for those with esophageal issues or swallowing problems.
“The improper administration of oral bisphosphonates can result in severe gastrointestinal side effects, stressing the importance of patient education and monitoring.”
Assessment of Patient Compliance Capability
Before starting bisphosphonate therapy, doctors should check if a patient can follow the upright posture rule. They look at the patient’s physical and mental health. If staying upright is hard, other treatments or intravenous bisphosphonates might be better.
Managing osteoporosis well means knowing the risks of bisphosphonates. Understanding the need for upright posture helps doctors make better choices for their patients.
Pregnancy and Lactation Considerations
Women of childbearing age taking bisphosphonates need to know about their pregnancy and lactation effects. Bisphosphonates stay in the bones for a long time. This could be a worry for the health of the fetus and baby.
FDA Pregnancy Category Classification
Bisphosphonates fall into certain FDA pregnancy categories. It’s important for doctors to understand these categories to make the right choices. The FDA looks at data on safety during pregnancy to decide these categories.
|
Bisphosphonate |
FDA Pregnancy Category |
|---|---|
|
Alendronate |
C |
|
Risedronate |
C |
|
Ibandronate |
C |
|
Zoledronic acid |
D |
The table shows most bisphosphonates are category C. This means animal studies show harm, but human studies are lacking. Zoledronic acid is category D, showing it’s risky for humans.
Long-term Skeletal Retention Concerns
Bisphosphonates stick to bones for a long time. This makes doctors worry about their release during pregnancy or breastfeeding. It could harm the fetus or baby.
“The long-term skeletal retention of bisphosphonates poses a unique challenge in managing osteoporosis in younger women who may become pregnant.”
Pre-conception Planning for Women of Childbearing Age
Women on bisphosphonates planning to get pregnant need to plan ahead. It’s key to talk about the risks and benefits with their doctor. They should weigh continuing treatment or stopping it before pregnancy.
We suggest women on bisphosphonates get their bone health checked often. If they’re planning to get pregnant, they might want to look into other treatments.
Conclusion: Balancing Benefits and Risks of Bisphosphonate Therapy
We’ve looked at how bisphosphonate therapy helps with osteoporosis. It makes bones stronger and lowers the chance of fractures. But, we must weigh its good points against the bad to manage osteoporosis well.
Bisphosphonates aren’t right for everyone. They’re not good for people with low calcium, kidney problems, stomach issues, or trouble staying upright. They’re also not safe for pregnant or breastfeeding women.
By thinking about these points and what each patient needs, we can make bisphosphonate therapy work best. It’s all about knowing the good and bad sides of this treatment to help patients with osteoporosis.
FAQ
What are bisphosphonates and how do they work in treating osteoporosis?
Bisphosphonates are medicines for osteoporosis. They stop bone loss, making bones stronger. They work by changing how bone cells break down.
What is the mechanism of action of nitrogen-containing bisphosphonates?
Nitrogen-containing bisphosphonates stop bone loss by blocking a key process in bone cells. This leads to the death of these cells, which is good for bones.
What are the clinical benefits of using bisphosphonates in osteoporosis management?
Bisphosphonates make bones denser and lower the chance of fractures. These benefits are key in fighting osteoporosis.
Why is hypocalcemia a contraindication for bisphosphonate therapy?
Bisphosphonates can lower calcium levels, which is bad for people with hypocalcemia. Doctors check calcium levels before and during treatment.
How does severe renal impairment affect the use of bisphosphonates?
Severe kidney problems can’t handle some bisphosphonates safely. Doctors use different rules for each drug. Sometimes, other treatments are better.
Can upper gastrointestinal disorders affect the use of oral bisphosphonates?
Yes, stomach and esophagus problems can make oral bisphosphonates risky. For those at high risk, doctors might choose intravenous options.
Why is the inability to maintain an upright posture a contraindication for oral bisphosphonates?
Not being able to sit up straight after taking oral bisphosphonates can hurt the esophagus. This is why it’s not safe.
Are bisphosphonates safe during pregnancy and lactation?
Bisphosphonates are not usually safe for pregnant or breastfeeding women. They stay in bones for a long time and could harm the baby. Women planning to have children should talk to their doctor first.
What are the indications for bisphosphonates in osteoporosis treatment?
Bisphosphonates are for men and women with osteoporosis, and those at high risk of breaking bones.
How do bisphosphonates impact bone mineral density and fracture risk?
Bisphosphonates make bones denser and lower fracture risk. This is important for managing osteoporosis.
References
National Center for Biotechnology Information. Evidence-Based Medical Guidance. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5409243/

































