Cerebral Amyloid Angiopathy (CAA) is a serious condition that affects the blood vessels in the brain. It leads to a significant decline in neurological function. It’s important for patients and their families to understand how CAA progresses and its impact end stage cerebral amyloid angiopathy.
CAA goes through several stages over 20 to 30 years. It causes severe cognitive and motor impairments. Thanks to new neuroimaging and care approaches, managing symptoms and improving life quality have become better.
Key Takeaways
- CAA is a progressive cerebrovascular disease with significant impact on life expectancy.
- Understanding the stages of CAA is key for managing symptoms and improving life quality.
- Advances in neuroimaging have improved diagnosis and treatment.
- Multidisciplinary care is vital for the best patient outcomes.
- Prognosis varies based on the stage and severity of CAA.
Understanding Cerebral Amyloid Angiopathy (CAA)

CAA is when amyloid proteins build up in brain blood vessel walls. This leads to cognitive decline and neurological symptoms, mainly in older adults.
Definition and Pathophysiology
Cerebral Amyloid Angiopathy is when amyloid proteins gather in brain blood vessels. This makes blood vessel walls weak, raising the risk of rupture and bleeding. The condition involves complex interactions between amyloid proteins and the brain’s vascular system.
The buildup of amyloid proteins in CAA harms normal blood flow to brain tissues. This can cause ischemic damage. Also, the blood vessels’ structure is weakened, increasing the chance of bleeding.
Prevalence and Risk Factors
CAA becomes more common with age, affecting many older people. Research shows CAA affects up to 30% of those aged 60-70 and over 50% of those over 90.
|
Age Group |
Prevalence of CAA |
|---|---|
|
60-70 years |
Up to 30% |
|
70-80 years |
40-50% |
|
Over 90 years |
More than 50% |
Factors that increase the risk of CAA include being older, having Alzheimer’s disease, and certain genetic traits. Knowing these risk factors helps in early detection and management of CAA.
The Four-Stage Progression of Cerebral Amyloid Angiopathy
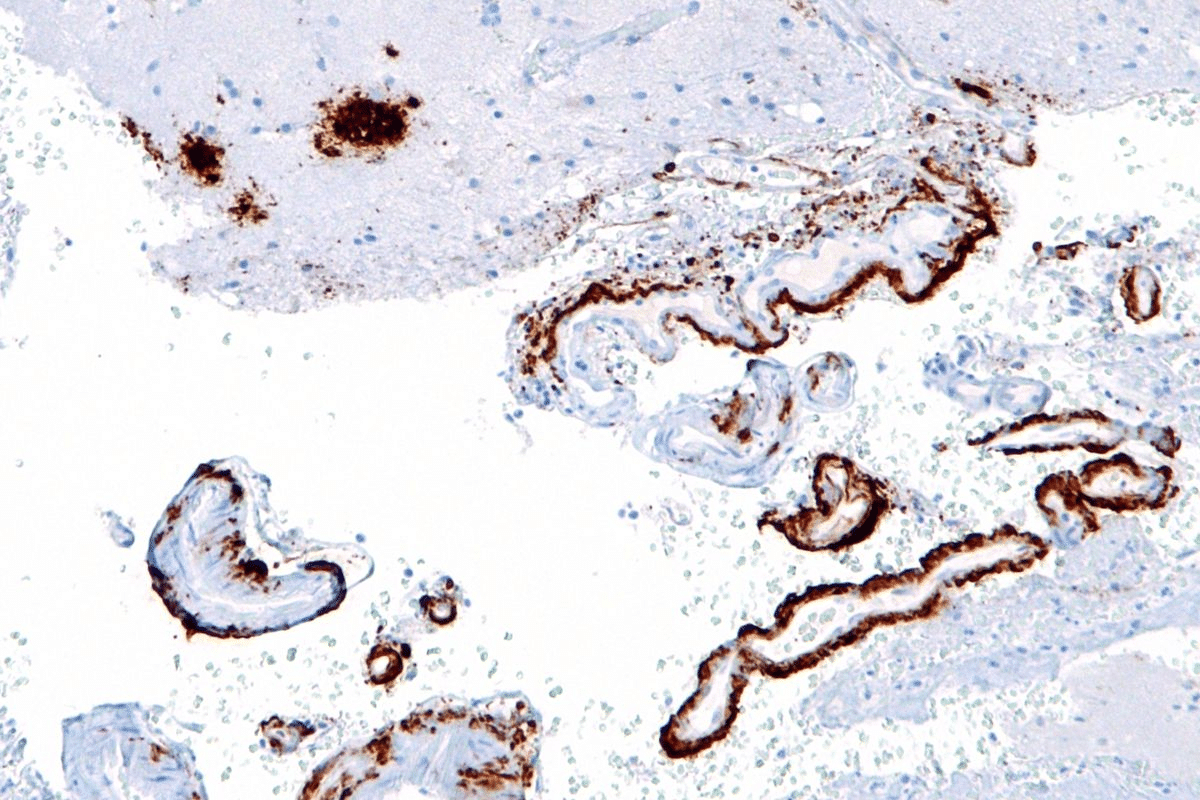
It’s important to know the stages of Cerebral Amyloid Angiopathy (CAA) for diagnosis and treatment. CAA happens when amyloid proteins build up in brain blood vessels. This causes changes in the brain.
Stage 1: Vascular Amyloid Deposition
In the first stage, amyloid proteins start to build up in blood vessel walls. This makes the walls thicker and can weaken them.
- Amyloid proteins accumulate in the vessel walls.
- Vessel wall thickening occurs, potentially leading to reduced vascular function.
Stage 2: Altered Cerebrovascular Physiology
The second stage changes how the brain’s blood vessels work. This can lead to poor blood flow and fragile vessels.
Key Features:
- Impaired vasodilation and vasoconstriction.
- Increased risk of vascular rupture.
Stage 3: Non-Hemorrhagic Brain Injury
In the third stage, CAA causes damage to brain tissue without bleeding. This can show up as white matter lesions or memory loss.
This damage can greatly affect a person’s life quality.
Stage 4: Hemorrhagic Brain Lesions
The final stage of CAA is marked by severe brain bleeding. These hemorrhages can be very dangerous.
Knowing these stages helps doctors manage CAA better. This can lead to better outcomes for patients.
Clinical Manifestations of CAA
CAA can show up in many ways, affecting the brain and nervous system.
The symptoms come from amyloid buildup in blood vessel walls. This buildup causes problems. Knowing these symptoms helps in managing the condition.
Cognitive Symptoms
Cognitive decline is a big part of CAA. It can look like dementia or mild cognitive impairment. Amyloid in blood vessels can cut off brain blood flow, causing brain problems.
People might struggle with memory, language, and solving problems. How fast these symptoms get worse can vary. Some people stay the same for a long time, while others get worse quickly.
Neurological Symptoms
CAA also causes neurological symptoms. These include seizures, stroke, and short-term brain problems. These symptoms often come from brain lesions caused by CAA.
Seizures can happen because of brain irritation from amyloid or bleeding. Stroke is another big symptom. It can happen when amyloid-filled vessels burst, causing bleeding in the brain.
|
Symptom Category |
Specific Symptoms |
Impact on Patients |
|---|---|---|
|
Cognitive Symptoms |
Memory loss, language difficulties, problem-solving challenges |
Impairs daily functioning, affects quality of life |
|
Neurological Symptoms |
Seizures, stroke, transient neurological deficits |
Can lead to acute neurological decline, increased morbidity |
End Stage Cerebral Amyloid Angiopathy: Defining the Final Phase
The final stage of cerebral amyloid angiopathy is very serious. It leads to a big drop in cognitive function and the formation of hemorrhagic brain lesions. This stage causes a lot of damage to the brain’s blood vessels, leading to severe symptoms.
Characteristic Features of End Stage CAA
End-stage CAA has several key features, including:
- Hemorrhagic Brain Lesions: These are a hallmark of advanced CAA, resulting from the rupture of amyloid-laden blood vessels.
- Cognitive Decline: Patients experience significant cognitive impairment, often manifesting as dementia.
- Neurological Symptoms: These can include seizures, stroke-like episodes, and other neurological deficits.
These features show the disease has advanced a lot. It’s important to have a good care plan and management strategies.
Differentiating from Other Neurodegenerative Conditions
It can be hard to tell end-stage CAA from other neurodegenerative diseases because their symptoms can be similar. But, there are some signs that can help:
- The presence of lobar hemorrhages, which are more typical of CAA.
- The absence of significant Alzheimer’s disease pathology in some cases.
- The presence of convexity subarachnoid hemorrhage, a condition often associated with CAA.
Getting the diagnosis right is key. It helps manage what patients expect and guides treatment choices.
Diagnosis and Assessment Methods
Getting a correct diagnosis of CAA is key. It uses neuroimaging techniques, specific clinical criteria, and biomarkers. Accurate diagnosis helps manage the condition better and improves patient outcomes.
Neuroimaging Techniques
Neuroimaging is vital for diagnosing CAA. MRI (Magnetic Resonance Imaging) and CT (Computed Tomography) scans help spot CAA’s signs. These include microbleeds, superficial siderosis, and white matter changes.
MRI is great because it shows blood products well. It finds hemorrhagic and non-hemorrhagic lesions linked to CAA. MRI’s gradient echo and susceptibility-weighted imaging make microbleeds and other lesions more visible.
Clinical Criteria and Biomarkers
Neuroimaging isn’t the only tool for diagnosing CAA. Clinical criteria and biomarkers are also key. The Boston criteria help classify CAA diagnosis as definite, probable, or possible.
Biomarkers, like amyloid-β peptides in cerebrospinal fluid, are being studied. They might help diagnose CAA better. Though not used in everyday practice yet, they show promise.
Using neuroimaging, clinical criteria, and biomarkers gives a full picture of CAA diagnosis. This helps doctors create the best treatment plans for patients.
Life Expectancy in Cerebral Amyloid Angiopathy
The life expectancy of people with cerebral amyloid angiopathy varies. It depends on the type of CAA they have.
Cerebral Amyloid Angiopathy (CAA) is a condition where amyloid proteins build up in brain blood vessels. This can cause neurological symptoms and greatly affect a person’s life quality.
Sporadic CAA Life Expectancy
Sporadic CAA is the most common type and is not passed down through genes. Life expectancy can vary a lot. It depends on things like other health issues, how bad the symptoms are, and how well treatment works.
People with sporadic CAA usually live shorter lives than others. Having bleeding in the brain and losing cognitive function are big risks for death.
Hereditary CAA Life Expectancy
Hereditary CAA, or familial CAA, is a rare form caused by genetic mutations. It often starts earlier and gets worse faster than sporadic CAA. Life expectancy can be different for each person.
The life span for those with hereditary CAA can vary a lot. It can be from the 40s to the 60s, depending on the genetic mutation and how the disease shows up.
|
CAA Type |
Average Life Expectancy |
Factors Influencing Life Expectancy |
|---|---|---|
|
Sporadic CAA |
Variable, often reduced compared to the general population |
Presence of comorbidities, severity of symptoms, effectiveness of management |
|
Hereditary CAA |
Ranges from 40s to 60s |
Specific genetic mutation, penetrance of the disease |
Knowing how long someone with CAA might live is important. It helps doctors and patients plan better. This can make life better for those with the condition.
Factors Influencing Prognosis in CAA
The outlook for Cerebral Amyloid Angiopathy (CAA) depends on age, health, and disease specifics. Knowing these factors helps predict outcomes and manage care.
Age and Comorbidities
Age is key in CAA prognosis. Older patients face a tougher time due to less health reserve and more comorbidities. Conditions like hypertension, diabetes, and heart disease can make things worse.
Having many health issues can affect treatment success and life quality for CAA patients. So, managing these conditions is vital in CAA care.
Hemorrhage Patterns and Severity
Hemorrhage type and severity greatly affect CAA prognosis. Lobar hemorrhages, common in CAA, can cause serious brain damage. How often and how much a patient bleeds is key to their outlook.
Those with more or bigger bleeds usually do worse than those with fewer or smaller ones. Keeping an eye on hemorrhage patterns and severity is important for predicting CAA outcomes.
Genetic and Environmental Factors
Genetics, like the APOE ε4 allele, can change CAA risk and prognosis. Genetic predisposition can influence when symptoms start and how severe they are.
Environmental factors, like lifestyle and exposure to risks, also impact prognosis. Understanding how genetics and environment interact can help find ways to prevent and treat CAA.
Management Strategies and Treatment Options
Managing CAA well needs a mix of today’s medicine and new treatments. This helps lessen symptoms and improve life quality for those affected.
Current Medical Approaches
Today, doctors mainly focus on controlling symptoms and preventing more damage. They manage high blood pressure, high cholesterol, and diabetes. These conditions can make CAA worse. Antihypertensive therapy is key because it helps keep blood pressure down and lowers the chance of bleeding.
Anticoagulant and antiplatelet therapies are used carefully in CAA patients. They can raise the risk of bleeding. Doctors decide on these treatments based on each patient’s situation, balancing benefits and risks.
|
Current Medical Approach |
Purpose |
Considerations |
|---|---|---|
|
Antihypertensive Therapy |
Reduce risk of hemorrhage |
Monitor blood pressure regularly |
|
Anticoagulant and Antiplatelet Therapies |
Prevent thrombotic events |
Use with caution due to hemorrhage risk |
Emerging Therapies and Clinical Trials
New research into CAA is promising. It includes immunotherapies targeting amyloid and other new ways to fight amyloid in blood vessels.
Clinical trials are key for checking if these new treatments are safe and work well. For example, some studies look at anti-amyloid antibodies to remove amyloid from blood vessels. This could lower the risk of bleeding and slow the disease.
The outlook for CAA treatment is bright with these new options. As research keeps going, we can expect even better treatments. This brings hope to those dealing with this tough condition.
Living with Cerebral Amyloid Angiopathy
It’s important to understand cerebral amyloid angiopathy (CAA) to help patients and their caregivers. CAA happens when amyloid proteins build up in brain blood vessels. This can cause cognitive and neurological symptoms.
Quality of Life Considerations
CAA can really affect a person’s life quality. It can cause cognitive decline, memory loss, and a higher risk of strokes. Symptoms range from mild cognitive issues to severe dementia.
The condition’s effects on life quality include:
- Cognitive Symptoms: Memory loss, confusion, and trouble with communication are common.
- Neurological Symptoms: Patients might have seizures, weakness, or paralysis.
- Emotional and Psychological Impact: Depression, anxiety, and mood swings are often seen.
Caregiving Challenges and Resources
Caring for someone with CAA is tough. Caregivers must handle physical care and emotional support. They need to manage the patient’s safety and emotional well-being.
Some big challenges for caregivers are:
- Managing daily care and ensuring patient safety.
- Coordinating medical appointments and treatments.
- Providing emotional support and coping with their own stress.
There are resources for caregivers:
- Support groups for sharing experiences and advice.
- Professional counseling services to manage stress and emotional challenges.
- Educational materials and workshops on caring for patients with CAA.
Understanding CAA’s challenges and using available resources helps caregivers. This improves the quality of life for both patients and caregivers.
Prevention and Risk Reduction
Preventing cerebral amyloid angiopathy (CAA) requires a mix of managing high blood pressure and living a healthy lifestyle. Knowing what increases the risk of CAA is key to preventing it.
Modifiable Risk Factors
There are several risk factors for CAA that can be changed to lower the risk. Hypertension is a big one that can be controlled to reduce CAA risk. Lifestyle choices and heart health also play a role.
|
Modifiable Risk Factor |
Impact on CAA Risk |
Intervention Strategies |
|---|---|---|
|
Hypertension |
High blood pressure can increase the risk of CAA by damaging blood vessels. |
Manage hypertension through medication, diet, and exercise. |
|
Smoking |
Smoking can damage vascular health, increasing the risk of CAA. |
Quit smoking through cessation programs and support. |
|
Physical Inactivity |
Lack of physical activity can contribute to overall poor cardiovascular health. |
Engage in regular physical activity, such as walking or other exercises. |
Lifestyle Interventions
Lifestyle changes are vital in lowering CAA risk. Eating a healthy diet full of fruits, veggies, and whole grains helps your blood vessels. Also, regular physical activity and keeping a healthy weight are key.
By tackling these changeable risk factors and living a healthy life, you can lower your chance of getting CAA. It’s important to work with your doctor to create a plan to prevent CAA.
Conclusion
Cerebral amyloid angiopathy (CAA) is a serious brain disease. It happens when amyloid beta peptides build up in the brain’s blood vessels. Knowing about CAA is key to diagnosing and treating it.
The final stage of CAA leads to big problems. People may lose their memory and face a higher risk of bleeding in the brain. This can shorten their life and make it less enjoyable.
Early detection and new treatments give hope for CAA patients. By learning about the risks and taking steps to prevent it, we can lower the chance of getting CAA.
Managing CAA well means using medicine, changing lifestyle habits, and getting support from caregivers. By studying CAA more, we can help patients live better lives and have a better outlook.
FAQ
What is cerebral amyloid angiopathy (CAA)?
Cerebral amyloid angiopathy (CAA) is a condition where amyloid protein builds up in brain blood vessels. This can cause various neurological symptoms and serious complications.
What are the stages of CAA progression?
CAA goes through four stages. First, amyloid deposits in blood vessels. Then, changes in blood vessel function. Next, brain injury without bleeding. Lastly, brain injury with bleeding.
What is the life expectancy for individuals with sporadic CAA?
Life expectancy for those with sporadic CAA varies. It depends on age, other health issues, and bleeding patterns. Generally, it’s lower than average.
How does CAA affect quality of life?
CAA can greatly reduce quality of life. It causes cognitive and neurological symptoms. It also raises the risk of severe strokes, leading to disability or death.
What are the characteristic features of end-stage CAA?
End-stage CAA shows severe cognitive decline and neurological impairment. It often includes repeated severe strokes, leading to a poor outlook.
How is CAA diagnosed?
Diagnosing CAA involves neuroimaging like MRI and CT scans. It also includes clinical criteria and biomarkers to spot amyloid in blood vessels.
What are the management strategies for CAA?
Managing CAA includes controlling blood pressure and managing other health issues. It also means avoiding certain medications. New treatments and trials aim to reduce amyloid deposits.
Can CAA be prevented?
While CAA can’t be fully prevented, some risk factors can be managed. This includes controlling high blood pressure and adopting a healthy lifestyle.
What is the difference between sporadic and hereditary CAA?
Sporadic CAA is the most common type, without a known genetic cause. Hereditary CAA is linked to specific genetic mutations, raising the risk of the condition.
How does age affect CAA prevalence?
Age is a major risk factor for CAA. The risk increases significantly after 60 years old.
What is the role of amyloid protein deposits in CAA?
Amyloid protein deposits in brain blood vessels are key to CAA. They cause blood vessel dysfunction, inflammation, and can lead to bleeding.
What are the caregiving challenges for individuals with CAA?
Caring for someone with CAA is challenging. It requires ongoing support due to the disease’s progressive nature and the need to manage symptoms.
Reference
National Center for Biotechnology Information. Evidence-Based Medical Guidance. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC9532921/



































