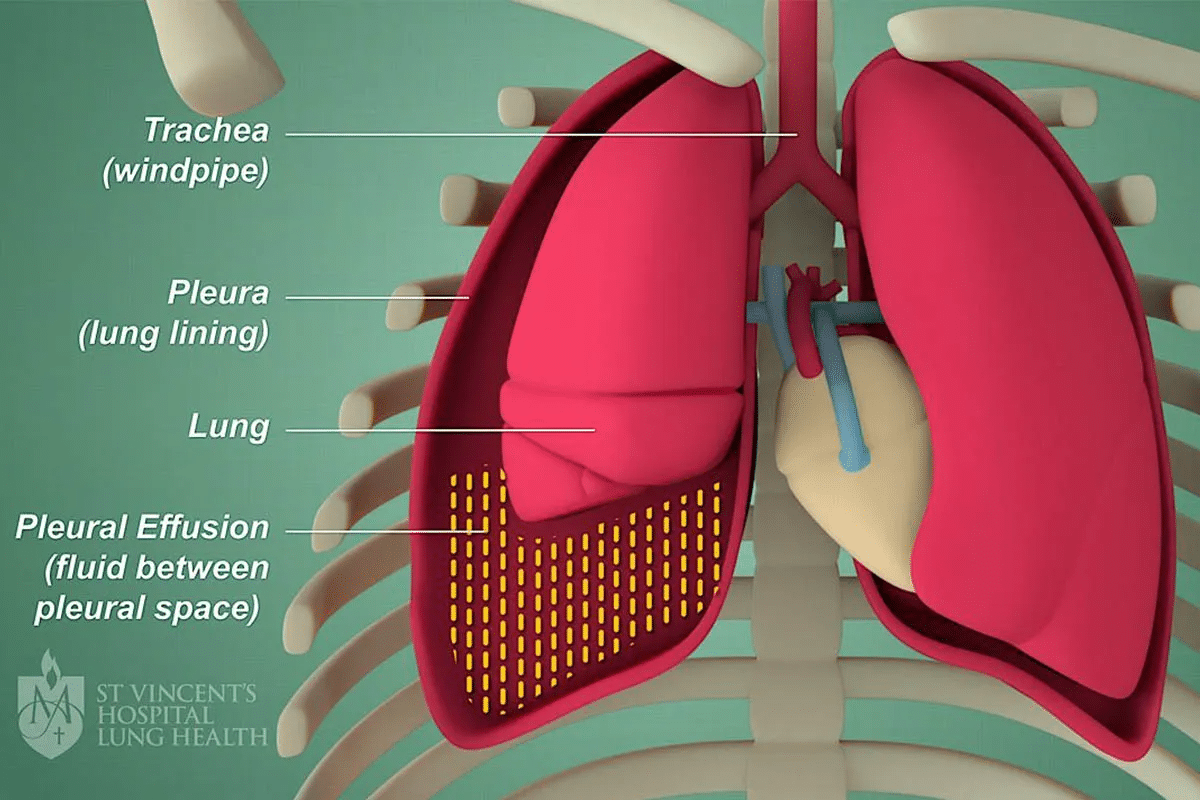
Chronic bronchitis is a long-term condition that makes the airways inflamed. It causes a persistent cough that brings up mucus. It’s a part of chronic obstructive pulmonary disease (COPD).chronic bronchitis pathophysiologyRespiratory Illness: Top 3 Most Dangerous Types
It’s important to understand the pathophysiology and etiology of this disease. At Liv Hospital, we use international medical knowledge and focus on the patient. This helps us give the best care and treatment plans.
Key Takeaways
- Chronic bronchitis is a form of COPD characterized by persistent productive cough.
- Understanding its pathophysiology and etiology is key to effective management.
- Liv Hospital offers complete care with international expertise and a patient-focused approach.
- Early recognition is vital for managing the disease well.
- There are effective strategies for managing chronic bronchitis.
Definition and Clinical Significance of Chronic Bronchitis
Chronic bronchitis is a big problem in respiratory diseases. It’s important to understand what it is and how it affects people. We’ll look at how it’s diagnosed and classified, and its connection to COPD and other lung issues.
Diagnostic Criteria and Classification
Chronic bronchitis is marked by a cough that lasts for at least 3 months in two years. This rule helps doctors spot it and tell it apart from other lung diseases.
To diagnose it, doctors look at your medical history and do a physical check-up. Chronic bronchitis can happen on its own or with COPD. Either way, it raises the chance of breathing problems and lung function loss.
Relationship to COPD and Other Respiratory Conditions
Chronic bronchitis often goes hand in hand with COPD. People with COPD and chronic bronchitis face a higher risk of worsening symptoms and a poorer outlook.
It can also show up with other lung diseases like asthma and bronchiectasis. This makes treating it more complex.
Epidemiology of Chronic Bronchitis
[Add image here]
It’s important to know about chronic bronchitis to help people. We look at how common it is, where it’s found, and who gets it. This helps us understand how big a problem it is.
Global Prevalence and Distribution
Chronic bronchitis hits about 3.4 to 22 percent of adults worldwide. It gets worse with age, smoking, work exposure, and lower income. The wide range in numbers shows how different places and people are affected.
|
Region |
Prevalence Rate (%) |
Primary Risk Factors |
|---|---|---|
|
North America |
5-10 |
Tobacco smoking, occupational exposure |
|
Europe |
4-12 |
Smoking, air pollution |
|
Asia |
3-15 |
Smoking, biomass fuel exposure |
Demographic Patterns and Risk Factors
Chronic bronchitis is not the same for everyone. It’s more common with age. Smoking is the biggest risk, making it worse.
Key demographic patterns and risk factors include:
- Age: Increasing prevalence with age
- Smoking status: Tobacco smoking as a major risk factor
- Occupational exposure: Dust and chemical fumes
- Socioeconomic status: Higher prevalence in lower socioeconomic groups
Knowing these patterns helps us focus our health efforts. We can aim to lessen the impact of chronic bronchitis.
Chronic Bronchitis Pathophysiology
To understand chronic bronchitis, we must look at airway inflammation and remodeling. This complex process involves many cellular and molecular interactions. These interactions lead to the disease’s characteristic symptoms.
Airway Inflammation and Remodeling
In chronic bronchitis, airway inflammation starts with the inhalation of irritants, like cigarette smoke. This triggers an immune response. Immune cells, such as macrophages and T lymphocytes, release inflammatory mediators.
These mediators, like cytokines and chemokines, cause inflammation and damage airways. The chronic inflammation causes airway remodeling. This includes thickening of the airway wall and an increase in smooth muscle mass.
These changes narrow the airways and limit airflow. This makes symptoms of chronic bronchitis worse.
Mucus Hypersecretion Mechanisms
Mucus hypersecretion is a key feature of chronic bronchitis. It results from the growth of goblet cells and mucous glands. This excessive mucus production blocks airways, making the disease harder to manage.
The production of mucus is a complex process. It involves epithelial cells, immune cells, and inflammatory mediators. In chronic bronchitis, the normal balance is disrupted, leading to too much mucus.
The changes in chronic bronchitis are connected. Airway inflammation leads to remodeling and mucus hypersecretion. Knowing these mechanisms is key to finding effective treatments.
Etiology: Primary Causes of Chronic Bronchitis
It’s important to know what causes chronic bronchitis to prevent and manage it well. This condition is influenced by many factors. These include lifestyle choices, what we’re exposed to, and our genes.
Tobacco Smoking and Nicotine Effects
Tobacco smoking is the main cause of chronic bronchitis. About 75 percent of those with the condition smoke or used to. Smoking harms our lungs, with nicotine and other chemicals causing inflammation and damage.
Smoking leads to chronic bronchitis through several ways. It increases mucus production, hampers ciliary function, and damages airway epithelium.
- Increased mucus production and secretion
- Impaired ciliary function
- Inflammation and damage to the airway epithelium
Environmental and Occupational Exposures
Environmental and job-related exposures also contribute to chronic bronchitis. Air pollutants like particulate matter, nitrogen dioxide, and sulfur dioxide irritate airways and cause chronic inflammation.
Jobs in mining, construction, and manufacturing expose workers to harmful substances. These can damage lungs and airways over time.
Genetic Predisposition and Host Factors
Genetics and host factors also affect chronic bronchitis. Certain genetic conditions, like alpha-1 antitrypsin deficiency, raise the risk of respiratory diseases.
Age, sex, and health conditions also play a part. Older adults and those with respiratory issues are more at risk from smoking and environmental exposures.
Cellular and Molecular Mechanisms
Chronic bronchitis is caused by many factors at the cellular and molecular level. We will dive into these to see how they affect the disease.
Goblet Cell Hyperplasia and Metaplasia
Goblet cell hyperplasia is a key feature of chronic bronchitis. It leads to too much mucus in the airways. This clogs the airways and makes symptoms worse.
Goblet cell metaplasia is when non-goblet cells turn into goblet cells. This makes even more mucus. It’s caused by inflammation and growth factors.
Inflammatory Mediators and Cytokines
Inflammatory mediators and cytokines are important in chronic bronchitis. They are released when the airways are injured or infected. They help start and keep the inflammation going, causing damage and changes in the airways.
Important ones include tumor necrosis factor-alpha (TNF-alpha), interleukin-8 (IL-8), and leukotriene B4 (LTB4). They bring more inflammatory cells, make more mucus, and make the airways more sensitive.
|
Inflammatory Mediator |
Role in Chronic Bronchitis |
|---|---|
|
TNF-alpha |
Promotes inflammation and airway damage |
|
IL-8 |
Attracts neutrophils to the airways |
|
LTB4 |
Contributes to airway inflammation and hyperresponsiveness |
Knowing how these mechanisms work is key to finding new treatments for chronic bronchitis.
Structural Changes in the Airways
Chronic bronchitis causes big changes in the airways. These changes affect how well the lungs work and how patients feel. The changes include more inflammation, more mucus, and changes in the airway structure.
Mucociliary dysfunction is a key part of chronic bronchitis. It’s how the body clears out bad stuff from the airways. But in chronic bronchitis, this process doesn’t work right because of mucus and cilia problems.
Mucociliary Dysfunction
Mucociliary dysfunction means the airways can’t clear mucus well. They make too much mucus that’s hard to move. Also, inflammation can damage the cilia, making it even harder to clear the airways.
Airway Wall Thickening and Fibrosis
Chronic bronchitis also makes the airway walls thicker because of fibrosis. This thickening is due to inflammation and the buildup of collagen. It narrows the airway, making breathing harder.
These changes make the disease worse and the outlook less good. Knowing about these changes helps us find better ways to treat chronic bronchitis and help patients.
These changes are complex and involve many factors. By understanding these, we can find new ways to fight the disease.
Clinical Manifestations and Symptoms
It’s key to know the symptoms of chronic bronchitis for right diagnosis and care. People with this condition often face many symptoms that affect their life quality.
Productive Cough and Sputum Characteristics
A key sign of chronic bronchitis is a chronic productive cough. This cough lasts at least three months in two years. The cough comes with sputum that can change in color and texture.
The sputum in chronic bronchitis is usually mucopurulent or purulent. This shows there are inflammatory cells and might mean a bacterial infection. The sputum’s volume and type can show how severe the disease is and if it’s getting worse.
Progression of Symptoms and Disease Staging
As chronic bronchitis gets worse, symptoms get more severe. This can lead to more dyspnea (shortness of breath) and less ability to exercise. The worsening of symptoms is tied to the disease’s stage, which is vital for choosing the right treatment.
Disease staging looks at how bad symptoms are, lung function, and how often the disease gets worse. We use systems like the GOLD criteria to stage COPD, which often goes with chronic bronchitis. Accurate staging helps doctors create treatment plans that fit each patient’s needs.
The symptoms of chronic bronchitis are complex and varied. A detailed assessment is key to managing the disease and helping patients get better.
Diagnostic Approaches and Assessment
We use a variety of methods to find chronic bronchitis. This includes both doctor’s opinions and advanced tests. Finding chronic bronchitis means looking at symptoms, medical history, and tests.
Clinical Evaluation and History Taking
First, we check symptoms like productive cough and sputum production. We also look at smoking history and exposure to harmful things. A full medical history helps us find risk factors and other health issues.
We also check for signs of trouble breathing, like wheezing or shortness of breath. This helps us decide what tests to do next.
Pulmonary Function Tests and Imaging Studies
Pulmonary function tests (PFTs) are key in diagnosing chronic bronchitis. Spirometry is a common test that checks forced expiratory volume in one second (FEV1) and forced vital capacity (FVC). These tests show how well air moves through the lungs.
Imaging tests like chest X-rays and computed tomography (CT) scans help rule out other problems. They show lung damage. These tests help confirm the diagnosis when combined with clinical findings and PFT results.
In summary, diagnosing chronic bronchitis needs a mix of doctor’s checks, history, tests, and imaging. Using these methods, we can accurately find and measure chronic bronchitis. This helps us choose the right treatment.
Treatment Strategies and Management
Managing chronic bronchitis needs a mix of treatments. We’ll look at how to reduce mucus, clear it out, and lower inflammation. This helps control the disease.
Pharmacological Interventions
Medicines are key in treating chronic bronchitis. Bronchodilators help open airways and improve breathing. Inhaled corticosteroids reduce swelling, which is good for those who often get worse.
We use different bronchodilators, like beta-2 agonists and anticholinergics. They can be used alone or together. The right medicine depends on how bad the symptoms are and how well the patient responds.
|
Medication Class |
Examples |
Primary Use |
|---|---|---|
|
Short-acting beta-2 agonists |
Albuterol, Salbutamol |
Quick relief of bronchospasm |
|
Long-acting beta-2 agonists |
Salmeterol, Formoterol |
Maintenance therapy to improve lung function |
|
Anticholinergics |
Ipratropium, Tiotropium |
Relaxation of airway smooth muscle |
Non-Pharmacological Approaches
There are also non-medical ways to manage chronic bronchitis. Pulmonary rehab programs help a lot. They include exercise, education, and changing behaviors.
Quitting smoking is very important. Smoking makes symptoms worse and speeds up the disease.
Emerging Therapies and Research Directions
New treatments for chronic bronchitis are being studied. These include anti-inflammatory drugs, mucolytics, and treatments that target specific disease pathways.
Personalized medicine is also being explored. It means tailoring treatments to each patient’s needs and genetic makeup.
Prevention and Risk Reduction
To lower the risk of chronic bronchitis, we need to know its causes. Then, we can use effective ways to prevent it. Understanding and preventing this condition is key to better health outcomes.
Smoking Cessation Programs
Stopping smoking is a big step in preventing chronic bronchitis. Smoking greatly increases the risk of getting this disease. Quitting can greatly lower this risk. We support programs that help people stop smoking.
Effective smoking cessation strategies include:
- Nicotine replacement therapy
- Prescription medications like bupropion or varenicline
- Counseling and behavioral therapy
- Support groups and hotlines
Occupational and Environmental Interventions
Workplace and environmental exposures also raise the risk of chronic bronchitis. We push for steps to lower these risks. This includes better air flow, protective gear, and cleaner air policies.
|
Intervention |
Description |
Benefit |
|---|---|---|
|
Improved Ventilation |
Enhancing airflow in workplaces and homes |
Reduces exposure to harmful particles |
|
Personal Protective Equipment (PPE) |
Using masks and respirators |
Filters out harmful dust and chemicals |
|
Air Pollution Policies |
Implementing regulations to reduce emissions |
Decreases ambient air pollution |
By using these prevention and risk reduction methods, we can make a big difference. Our approach covers both personal actions and environmental changes.
Conclusion
Understanding chronic bronchitis is key to managing the disease well. We’ve looked into what it is, why it matters, and how to diagnose it. We’ve also seen how it connects to other lung problems.
Chronic bronchitis is a complex issue. It involves inflammation, too much mucus, and changes in airways. Smoking and environmental factors are big causes. We talked about the best ways to treat it, including medicines and lifestyle changes.
In short, managing chronic bronchitis needs a full approach. Knowing the disease’s causes and how it works helps doctors give better care. This improves patients’ lives and health.
FAQ
What is chronic bronchitis?
Chronic bronchitis is a lung disease. It causes long-term inflammation and irritation in the bronchial tubes. This leads to a persistent cough and mucus production.
What are the primary causes of chronic bronchitis?
Main causes include smoking, exposure to pollutants, and genetics. These factors can damage the lungs and airways.
How is chronic bronchitis diagnosed?
Doctors use several methods to diagnose it. These include clinical evaluation, pulmonary function tests, and imaging studies like chest X-rays and CT scans.
What are the symptoms of chronic bronchitis?
Symptoms include a productive cough, mucus production, wheezing, and shortness of breath. These symptoms can get worse if not treated properly.
How is chronic bronchitis treated?
Treatment involves medications like bronchodilators and corticosteroids. It also includes non-pharmacological approaches and lifestyle changes, such as quitting smoking.
Can chronic bronchitis be prevented?
Yes, it can be prevented or slowed down. This is done through smoking cessation programs, occupational and environmental interventions, and avoiding pollutants.
What is the relationship between chronic bronchitis and COPD?
Chronic bronchitis is a type of COPD. It often comes with emphysema. Understanding this relationship is key to effective management and treatment.
What is the pathophysiology of chronic bronchitis?
It involves airway inflammation, remodeling, and mucus hypersecretion. This leads to chronic cough, mucus production, and can cause airflow limitation and respiratory failure.
How does smoking affect chronic bronchitis?
Smoking is a major risk factor. It damages the lungs and airways, causing chronic inflammation and irritation. This increases the risk of COPD.
What is the role of goblet cells in chronic bronchitis?
Goblet cells are key in chronic bronchitis. They produce mucus, which can become excessive. This contributes to symptoms and disease progression.
What are the clinical features of chronic bronchitis?
Symptoms include a productive cough, mucus production, wheezing, and shortness of breath. These can vary in severity and impact quality of life.
How does chronic bronchitis affect lung function?
It can lead to airflow limitation and reduced lung function. This makes breathing harder and can result in respiratory failure if not treated properly.
References
ational Center for Biotechnology Information. Evidence-Based Medical Guidance. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK179276/
































