
Chemotherapy is a lifesaving treatment for many cancer patients. But, it can weaken bones and raise the risk of osteoporosis. This serious side effect can harm quality of life long after treatment ends. It can lead to devastating fractures and loss of mobility osteoporosis cancer.
Studies show that chemotherapy and radiation can cause bone loss. This increases the risk of fractures. About 70% of patients dying from cancer experience bone loss. This is a big health problem.
It’s important to understand how chemotherapy affects bone health. This knowledge helps manage the health of cancer patients.
Key Takeaways
- Chemotherapy can lead to bone loss and increased fracture risk.
- Osteoporosis is a significant health concern for cancer survivors.
- Exposure to chemotherapy and radiation can cause bone loss.
- Understanding the link between chemotherapy and bone health is important.
- Cancer patients are at risk for osteoporosis, specially with certain treatments.
The Link Between Cancer Treatment and Bone Health
Cancer treatment can harm bone health, leading to osteoporosis. Our bones are always changing, thanks to bone-building and bone-resorbing cells. But, cancer treatments can upset this balance.
Understanding Bone Density and Strength
Bone density is how much minerals like calcium are in your bones. More minerals mean stronger bones that break less easily. “The condition develops when bones become weak and brittle, characterized by low bone density that makes bones more susceptible to breaking,” as noted by medical experts. Keeping bone density high is key, even for those with cancer.
Bones are always being renewed through bone remodeling. This process removes old bone and adds new one. But, some cancer treatments can mess with this, causing bone loss.
How Cancer Treatments Affect Bone Metabolism
Cancer treatments, like chemotherapy and hormone therapy, can harm bone metabolism. Chemotherapy can directly harm bone cells. Hormone therapy can change hormone levels, affecting bone density. For example, therapies that lower estrogen can speed up bone loss, as estrogen helps keep bones strong.
It’s vital to understand how cancer treatments affect bones. This knowledge helps doctors manage bone health in cancer patients. By knowing the risks, healthcare providers can take steps to protect bone health.
“The link between cancer treatment and bone health is complex and multifaceted, requiring a comprehensive approach to manage and prevent long-term complications.”
Patients and doctors need to be aware of bone health risks from cancer treatment. This way, they can work together to reduce these risks and improve overall health.
What is Osteoporosis and How Does it Develop?
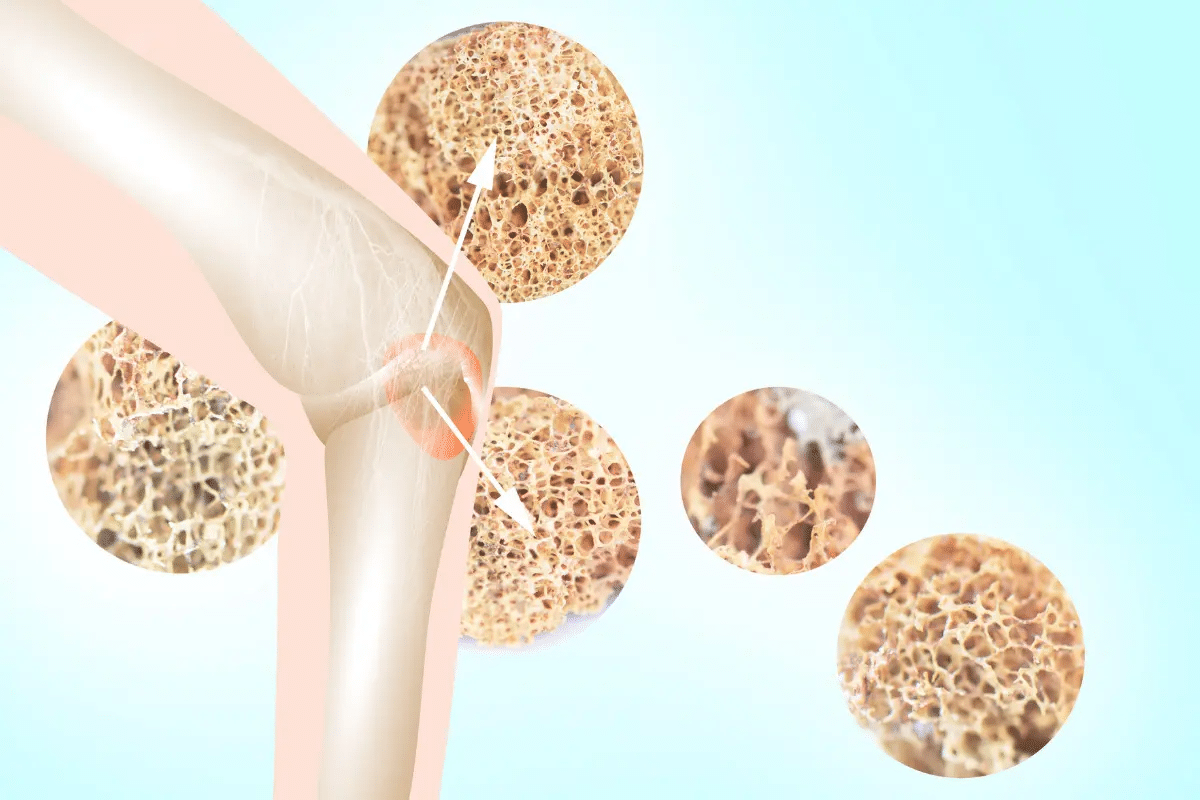
Let’s dive into how chemotherapy affects bones. First, we need to know what osteoporosis is and how it starts. Osteoporosis makes bones weak and brittle because of low bone density. It happens when the body can’t keep up with bone loss and formation.
Definition and Characteristics of Osteoporosis
Osteoporosis occurs when the body loses more bone than it can make. This results in thinner and weaker bones. About 70% of cancer patients suffer from bone loss, which is a big problem.
Normal Bone Remodeling Process
Bones are always being rebuilt through a cycle of breakdown and formation. This keeps bones healthy and strong. But in osteoporosis, this cycle gets out of balance, leading to bone loss.
Pathophysiology of Bone Loss
Bone loss in osteoporosis comes from complex cell and hormone actions. When bone breakdown and formation aren’t balanced, bone density drops. This imbalance can be caused by cancer treatment, hormonal changes, and lifestyle choices.
Knowing how bones are remade and how osteoporosis affects this is key. It helps us find ways to prevent and treat the condition. By understanding osteoporosis and its causes, doctors can help patients better.
The Prevalence of Osteoporosis Cancer Among Chemotherapy Patients
Research shows that some chemotherapy drugs can lower bone density, raising the risk of osteoporosis. This is a big worry because osteoporosis can cause fractures and other issues that harm cancer survivors’ quality of life. We will look at the stats and research on osteoporosis in chemotherapy patients. We will also find out which cancers are more likely to cause bone loss.
Statistical Evidence and Research Findings
Studies have found that chemotherapy can cause bone loss. For example, a study in the Journal of Clinical Oncology found that women with breast cancer who had chemotherapy lost a lot of bone density. Drugs like doxorubicin, paclitaxel, and cisplatin contribute to this loss by lowering calcium levels and disrupting bone cells.
The risk of osteoporosis in chemotherapy patients varies by cancer type and treatment. For instance, those with breast cancer and prostate cancer are at higher risk. This is because their treatments, like hormonal therapies, can speed up bone loss.
|
Cancer Type |
Chemotherapy Drugs Used |
Risk of Osteoporosis |
|---|---|---|
|
Breast Cancer |
Doxorubicin, Paclitaxel |
High |
|
Prostate Cancer |
Cisplatin, Docetaxel |
High |
|
Lymphoma |
Cyclophosphamide, Doxorubicin |
Moderate |
High-Risk Cancer Types for Bone Density Loss
Some cancers and their treatments are more likely to cause bone loss. For example, breast cancer and prostate cancer treatments often involve hormonal therapies that can lead to faster bone loss. Also, cancers that spread to the bone, like lung and thyroid cancer, can increase osteoporosis risk because tumor cells harm bone tissue.
Knowing these risks is key to creating better prevention and treatment plans for chemotherapy patients. By identifying high-risk cancers and the drugs used, doctors can take steps to protect bone health.
Mechanisms of Chemotherapy-Induced Bone Loss
Chemotherapy can harm bone density in many ways. It affects bone cells and how bones are made and broken down. Knowing how it works helps find ways to stop bone loss in chemo patients.
Direct Effects on Bone Cells
Chemotherapy drugs can harm bone cells. This leads to an imbalance in how bones are made and broken down. This imbalance causes bones to lose density over time.
Research has shown that some chemo drugs slow down bone-making cells but speed up bone-breaking cells. This makes bones weaker and more likely to break.
Calcium Depletion Mechanisms
Chemotherapy can also make bones weak by depleting calcium. Calcium is key for strong bones. Without enough, bones get weaker and more prone to fractures.
How chemo drugs cause calcium loss is complex. Some drugs can cause early menopause in women. This leads to a drop in estrogen, which helps keep bones strong. Losing estrogen increases the risk of osteoporosis.
Cellular Senescence and Bone Remodeling
Chemotherapy can also lead to bone loss through cellular senescence. Senescent cells stop dividing but keep working. They can mess with bone remodeling by releasing factors that harm bone health.
This explains why chemo can cause more bone loss than hormone therapy. Understanding senescence in chemo-induced bone loss helps find new treatments.
Knowing how chemo affects bones helps doctors prevent and treat bone loss better. They can check bone density, manage calcium, and use drugs to protect bones during chemo.
Specific Chemotherapy Drugs That Impact Bone Density
Chemotherapy can harm bone health, with some drugs causing bone loss. Certain drugs have a big impact on bone density. This can lead to osteoporosis and higher fracture risk in cancer patients.
Doxorubicin and Its Effects on Bone Health
Doxorubicin is a common chemotherapy drug used for many cancers. It’s effective but can harm bone health. Research shows it can cause bone loss by affecting bone cells and disrupting bone remodeling.
Key effects of doxorubicin on bone health include:
- Decreased bone formation due to the suppression of osteoblast activity
- Increased bone resorption resulting from the stimulation of osteoclasts
- Disruption of the balance between bone formation and resorption
Paclitaxel’s Impact on Bone Structure
Paclitaxel is used to treat ovarian, breast, and lung cancers. It can harm bone structure and density. It affects bone health by changing bone cell function and promoting bone resorption.
The ways paclitaxel affects bone health are complex. It involves:
- Induction of cellular stress and damage in bone cells
- Alteration of the microenvironment within bone tissue
- Potential hormonal changes that contribute to bone loss
Cisplatin and Other Platinum-Based Compounds
Cisplatin is used to treat testicular, ovarian, and bladder cancers. It can harm bone health, leading to long-term bone density loss in survivors.
The impact of cisplatin on bone health may be due to:
- Direct toxic effects on bone cells
- Induction of oxidative stress and inflammation within bone tissue
- Hormonal changes, including chemotherapy-induced menopause in women, which can accelerate bone loss
Chemotherapy-induced menopause is a big concern. It can lead to a quick drop in estrogen levels, worsening bone loss. This is a big worry for breast cancer treatments, where bone density loss is a risk.
Hormonal Changes: Chemotherapy-Induced Menopause and Bone Loss
Chemotherapy can cause menopause in women, raising their risk of osteoporosis. This is because estrogen loss speeds up bone loss. Estrogen is key to keeping bones strong.
Estrogen Depletion and Accelerated Bone Loss
Estrogen helps bones by making them and keeping them from breaking down. When estrogen drops due to chemotherapy, bones start to lose mass faster. Studies show women who get menopause early from chemo are more likely to get osteoporosis.
Key factors contributing to estrogen depletion and bone loss include:
- Reduced estrogen production
- Increased bone resorption
- Decreased bone formation
Premature Menopause in Female Cancer Patients
Chemotherapy often leads to early menopause in women with cancer. Research shows these women tend to get menopause sooner. This can harm their bones over time.
The impact of premature menopause on bone health is multifaceted:
- Increased risk of osteoporosis
- Accelerated bone loss
- Higher risk of fractures
Hormonal Mechanisms of Bone Deterioration
The way bones deteriorate due to chemotherapy-induced menopause involves many hormones and bone cells. Knowing this helps in finding ways to stop or slow bone loss in cancer patients.
Healthcare providers can take steps to lessen these risks. This helps improve the health and well-being of female cancer survivors.
Risk Factors for Developing Chemotherapy-Related Osteoporosis
It’s important to know the risk factors for osteoporosis during chemotherapy. This knowledge helps in preventing and managing the condition. Several factors can increase the risk, and knowing them can help reduce these risks.
Pre-existing Bone Health Conditions
People with existing bone health issues are more likely to get osteoporosis from chemotherapy. Conditions like osteopenia or past fractures can make bones weaker. This makes them more vulnerable to chemotherapy’s effects.
Age and Gender Considerations
Age and gender are key in bone health. Older adults and postmenopausal women are more at risk. This is because of natural bone loss with age and hormonal changes. Chemotherapy can make this risk even higher.
Cancer Type and Treatment Protocol
The type of cancer and treatment can affect the risk of osteoporosis. Some cancers and treatments, like hormonal therapies or certain chemotherapies, can harm bone density.
Lifestyle and Nutritional Factors
Lifestyle and diet also play a part in osteoporosis risk. Smoking, physical inactivity, and a diet lacking calcium and vitamin D can weaken bones. This makes them more vulnerable to chemotherapy’s effects.
Healthcare providers can use this knowledge to prevent or manage osteoporosis in cancer patients. This can greatly improve their quality of life.
Long-Term Consequences: Fracture Risks and Complications
Chemotherapy can harm bone health in cancer survivors. It’s vital to focus on bone density and quality of life as we fight cancer. This helps improve treatment outcomes.
Increased Fracture Susceptibility
Osteoporosis is often called a “silent disease” because it doesn’t show symptoms until a fracture happens. The side effects of osteoporosis can greatly reduce quality of life. Bones become weak and brittle, making them more likely to break.
Impact on Cancer Survivorship
Chemotherapy-induced osteoporosis can greatly affect cancer survivors. Fractures and bone issues can limit movement, cause chronic pain, and worsen health. It’s key to watch and manage bone health during and after treatment.
Quality of Life Considerations
The bone thinning symptoms of osteoporosis can deeply affect a person’s life. Simple tasks become hard, and the fear of fractures can cause anxiety and loss of independence. We need to think about these when helping cancer survivors.
Understanding the long-term effects of chemotherapy-induced osteoporosis helps us improve life for cancer survivors. We must tackle fracture risks, monitor bone health, and offer full support to those affected.
Monitoring and Diagnosing Bone Health During Cancer Treatment
Cancer treatment has made great strides, but keeping an eye on bone health is more important than ever. Cancer patients need to have their bones checked regularly. This helps prevent osteoporosis and keeps them healthy.
Bone Density Testing Methods
Bone density tests are key for watching over bone health during cancer treatment. The most used test is the DEXA (dual-energy X-ray absorptiometry) scan, or DXA scan. It’s a safe test that uses a tiny bit of radiation to check bone mineral content.
DEXA scans help in many ways:
- They measure bone mineral density (BMD)
- They help diagnose osteoporosis
- They track changes in bone density over time
Recommended Screening Protocols
Screening for bone density depends on several factors like age, gender, and risk. Here’s what we recommend:
- Start with a DEXA scan at the beginning of treatment
- Have follow-up scans every 1-2 years, based on risk
- Check more often if you’re on high-risk treatments or have had fractures
Warning Signs and Symptoms
Knowing the signs of osteoporosis is vital for catching it early. Look out for:
- Back pain from vertebral fractures
- Loss of height over time
- Stooped posture or a curved spine
- Frequent fractures with little trauma
Spotting these signs early can greatly help manage osteoporosis. It can also improve the life quality of cancer patients.
Prevention and Treatment Strategies for Chemotherapy-Induced Bone Loss
Managing bone loss from chemotherapy involves nutrition, exercise, and medicine. A mix of these methods is key to keeping bones strong during cancer treatment.
Nutritional Interventions
Eating right is vital to stop osteoporosis during chemo. You need enough calcium and vitamin D to keep bones dense. A diet full of dairy, leafy greens, and fortified foods is best.
For those who can’t get enough from food, supplements might help. But always talk to a doctor before taking any supplements to avoid side effects.
Exercise and Physical Activity Guidelines
Exercise is essential for bone health and feeling good during chemo. Weight-bearing exercises like walking or jogging are great for bones. They also help with balance.
Adding exercises that improve flexibility and balance is also important. This can help prevent falls and fractures. Always work with your healthcare team to create a safe and effective exercise plan.
Pharmacological Options
If you’re at high risk of bone loss from chemo, medicine might be needed. Bisphosphonates help by stopping bone breakdown and making bones stronger. Denosumab is another option, depending on your situation.
Talking to your doctor about these medicines is important. They can help you understand the benefits and risks.
Integrative Approaches to Bone Health
Combining medical treatments with lifestyle changes is a powerful way to manage bone health. A holistic lifestyle includes a balanced diet, regular exercise, managing stress, and enough sleep.
By being proactive and using a variety of methods, you can lower your risk of bone loss. This helps keep you healthy and feeling good.
Conclusion
It’s important for cancer survivors to understand the link between chemotherapy and osteoporosis. Chemotherapy-induced osteoporosis is a big health issue that needs attention and action. Taking care of your bones is key to staying healthy and enjoying life while fighting cancer.
Some chemotherapy treatments raise the risk of osteoporosis. It’s critical to watch your bone health closely. By knowing the risk factors and using prevention and treatment plans, survivors can lower their osteoporosis risk.
We stress the need for a full approach to bone health. This includes good nutrition, exercise, and medicine. By being proactive, survivors can live better lives and avoid fractures and other bone problems linked to chemotherapy and osteoporosis.
FAQ
Can chemotherapy cause osteoporosis?
Yes, chemotherapy can lead to osteoporosis. It disrupts the balance between bone-building and bone-dismantling cells. This results in bone loss and a higher risk of fractures.
What is osteoporosis?
Osteoporosis is a condition where bones become weak and brittle. This makes them more likely to break.
How does chemotherapy affect bone density?
Chemotherapy drugs can harm bone cells and lower calcium levels. They also cause cells to stop growing. This leads to bone loss and an imbalance in bone remodeling.
Which chemotherapy drugs impact bone density?
Certain drugs like doxorubicin, paclitaxel, and cisplatin can harm bone health. They cause bone loss.
Does chemotherapy-induced menopause accelerate bone loss?
Yes, menopause caused by chemotherapy can speed up bone loss in women. This is because estrogen helps keep bones strong.
What are the risk factors for developing chemotherapy-related osteoporosis?
Risk factors include pre-existing bone health issues, age, gender, and cancer type. Treatment protocol, lifestyle, and nutrition also play a role.
How can chemotherapy-induced bone loss be prevented or treated?
To prevent or treat bone loss, focus on nutrition, exercise, and certain medications like bisphosphonates. Integrative approaches to bone health are also important.
What are the long-term consequences of chemotherapy-induced osteoporosis?
Long-term effects include a higher risk of fractures and impacts on cancer survivorship. It also affects quality of life.
How is bone health monitored during cancer treatment?
Bone health is checked through bone density tests and screening protocols. It’s also important to be aware of warning signs and symptoms.
Is osteoporosis caused by cancer or chemotherapy?
Osteoporosis can be caused by both cancer and chemotherapy. Certain cancers and treatments can disrupt bone metabolism, leading to bone loss.
Can lifestyle and nutritional factors influence bone health during chemotherapy?
Yes, lifestyle and nutrition can affect bone health. It’s important to get enough calcium and vitamin D to maintain bone density.
Reference
National Center for Biotechnology Information. Chemotherapy-Induced Osteoporosis: Risk and Long-Term Impact. Retrieved fromhttps://pmc.ncbi.nlm.nih.gov/articles/PMC10004442/



































