
Pneumococcal pneumonia is a serious lung infection caused by Streptococcus pneumoniae bacteria. This pathogen is a major cause of illness and death worldwide. It leads to about 1.6 million deaths each year globally.pneumococcal pneumonia treatment5 Things to Expect After Your Last Chemo Treatment: Recovery and Beyond
At Liv Hospital, we focus on giving the best care for this serious infection. We use the latest diagnostic tools and tailor treatment protocols for each patient. Our goal is to get the best results and care for our patients.
Key Takeaways
- Understanding pneumococcal pneumonia causes and symptoms is key for effective management.
- Quick diagnosis and treatment can greatly improve patient outcomes.
- Antibiotic therapies and supportive care are vital for treating pneumococcal pneumonia.
- Customized treatment plans help fight antibiotic resistance.
- Putting the patient first is essential for the best medical results.
Understanding Pneumococcal Pneumonia
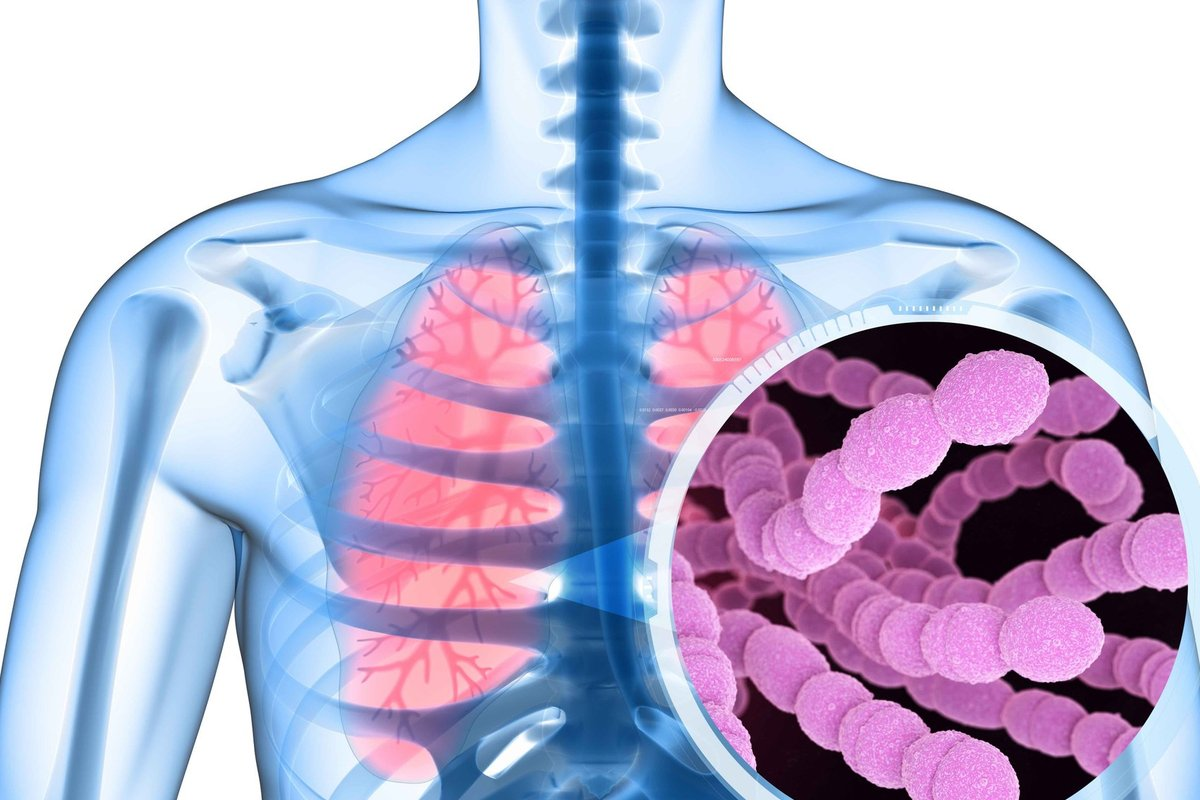
Fighting pneumococcal pneumonia starts with knowing the disease well. It’s caused by Streptococcus pneumoniae. Knowing this helps create better treatment plans and improves patient care.
What is Pneumococcal Pneumonia?
Pneumococcal pneumonia is an infection of the lungs by Streptococcus pneumoniae. This bacterium can cause infections ranging from mild to severe. These include pneumonia, meningitis, and sepsis.
The disease’s severity varies. It depends on age, health, and any underlying conditions.
The Role of Streptococcus pneumoniae
Streptococcus pneumoniae is a Gram-positive bacterium found in the upper respiratory tract. It can be harmless but becomes dangerous under certain conditions. Its ability to infect the lungs is key in causing pneumococcal pneumonia.
Understanding Streptococcus pneumoniae is vital. It helps in creating targeted treatments and interventions.
Pathophysiology and Disease Progression
The disease starts when Streptococcus pneumoniae invades lung tissue. This leads to inflammation and infection. Symptoms can worsen quickly.
Knowing how the disease progresses is key. It helps in finding effective treatments and improving patient care.
As the disease gets worse, it can cause serious complications. These include bacteremia, meningitis, and respiratory failure. It’s important to recognize these risks to provide the right care.
Epidemiology and Global Impact
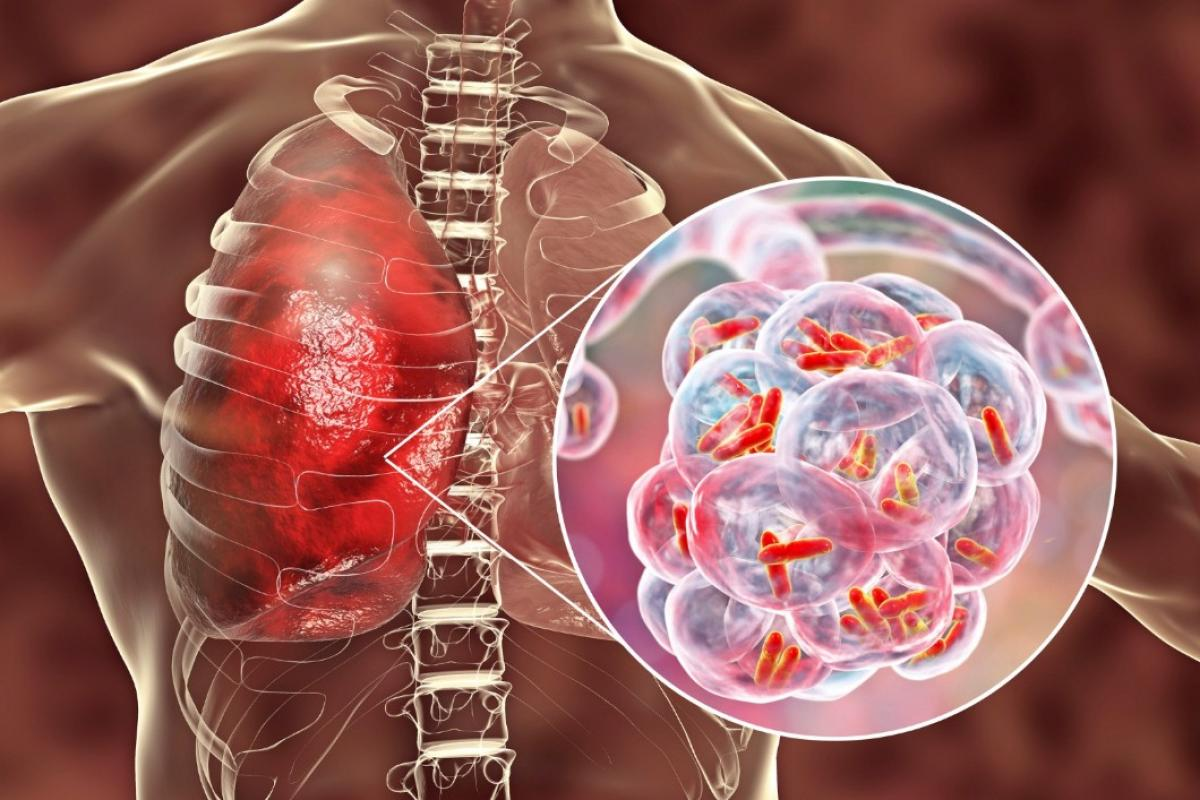
Understanding pneumococcal disease is key to fighting it. It affects people worldwide, with different rates of illness and death. This varies by region and population.
Worldwide Prevalence and Mortality Statistics
Pneumococcal infections are a big problem globally. They cause about 1.6 million deaths each year. Most of these deaths happen in poor countries where healthcare is scarce.
The number of cases usually goes up in winter, peaking in December and January. Knowing this helps doctors treat pneumococcal disease better.
Key Statistics:
- 1.6 million deaths annually due to pneumococcal infections
- Higher mortality rates in low-income countries
- Seasonal peak in winter months (December and January)
Demographic Distribution
Pneumococcal disease hits different groups hard. Young children, older adults, and those with health issues are at higher risk.
This shows why we need to focus our efforts. Vaccines, like pneumococcal conjugate vaccines (PCVs), are very effective in kids.
Economic Burden of Pneumococcal Disease
The cost of pneumococcal disease is huge. It includes direct healthcare costs and lost productivity. In the U.S., it costs billions every year.
By reducing cases through vaccines and prevention, we can save money. We must keep funding research and public health efforts to fight pneumococcal disease.
Risk Factors and Vulnerable Populations
Not everyone is at the same risk for pneumococcal pneumonia. Some groups face higher risks due to different factors. Knowing these risks helps us find who needs extra care and how to help them.
Age-Related Risks
Age is a big factor in getting pneumococcal pneumonia. Young kids and older adults are more at risk. Kids under 2 have weaker immune systems, while older adults’ immune strength drops with age.
Studies show that pneumococcal disease can be deadly, with death rates up to 30% in the elderly. This shows how critical it is to watch over these groups closely and act fast when needed.
Comorbidities and Predisposing Conditions
Some health issues make people more likely to get pneumococcal pneumonia. Heart disease, diabetes, and lung problems are examples. Also, those with weakened immune systems, like those with HIV/AIDS or on immunosuppressive drugs, are at higher risk.
People with weak immune systems are most likely to get pneumococcal infections. This makes it important to take extra steps to protect them.
Environmental and Lifestyle Factors
Environmental and lifestyle choices also affect pneumococcal pneumonia risk. Smoking and air pollution harm lungs and make infections more likely. Living in crowded places or areas with poor healthcare also raises the risk.
“Prevention is key, specially for those at high risk. Vaccines and lifestyle changes are important steps in prevention, along with managing health conditions.”
By tackling these risk factors, we can shield vulnerable groups and lower pneumococcal pneumonia cases.
Clinical Presentation and Symptoms
Knowing the symptoms of pneumococcal pneumonia is key for early treatment. This illness can show mild to severe signs. It’s important to know both common and severe symptoms.
Common Symptoms
Pneumococcal pneumonia often brings a high fever, aches, headache, and feeling unwell. These symptoms can change in intensity and appear quickly.
- Fever, often accompanied by chills
- Cough, which may be productive or non-productive
- Shortness of breath or difficulty breathing
- Chest pain or discomfort that worsens with coughing or deep breathing
- Fatigue and weakness
Severe Manifestations
In serious cases, pneumococcal pneumonia can cause severe problems. These include:
- Respiratory failure needing a ventilator
- Septic shock, with low blood pressure and organ failure
- Multi-organ dysfunction
These severe issues need quick medical help and often require hospital care.
Differentiating from Other Respiratory Infections
It’s hard to tell pneumococcal pneumonia from other respiratory infections because symptoms can be similar. But, some signs can help diagnose it:
- The presence of high fever and rigors
- The nature of the cough and sputum production
- Associated symptoms such as headache and muscle pain
Red Flags Requiring Immediate Medical Attention
Some symptoms and signs need quick medical check-up, including:
- Difficulty breathing or shortness of breath
- Chest pain or pressure
- Coughing up blood or rust-colored mucus
- Confusion or disorientation
- Severe headache or stiff neck
Spotting these red flags is vital for quick action and avoiding worse problems.
Diagnostic Approaches
Diagnosing pneumococcal pneumonia requires a detailed approach. This includes physical exams, lab tests, and imaging studies. Getting the diagnosis right is key to treating the disease effectively.
Physical Examination Findings
A thorough physical exam is the first step. We look for fever, fast breathing, and a fast heart rate. We also check for consolidation in the lungs, which sounds like crackles or bronchial breath sounds.
These signs guide us to further tests and help us understand how severe the disease is.
Laboratory Tests
Laboratory tests are vital in confirming pneumococcal pneumonia. Common tests include:
- Complete Blood Count (CBC): To check for increased white blood cells, a sign of bacterial infection.
- Blood Cultures: To find the cause of the infection.
- Pneumococcal Urinary Antigen Test (UAT): A quick test for pneumococcal antigen in urine.
These tests help confirm Streptococcus pneumoniae and guide antibiotic treatment.
Imaging Studies
Imaging studies, like chest X-rays, are key for diagnosing pneumococcal pneumonia. We look for:
- Lobar consolidation, a sign of pneumococcal pneumonia.
- Possible pleural effusion.
Chest X-rays help us see how much of the lung is affected and spot any complications.
Microbiological Confirmation Methods
Confirming the diagnosis involves several methods, including:
- Sputum Gram Stain and Culture: To identify the cause.
- Blood Cultures: Important for detecting bacteremia.
- Pneumococcal Antigen Detection: Tests like UAT for quick diagnosis.
These methods are essential for confirming the diagnosis and tailoring treatment.
Pneumococcal Pneumonia Treatment: Current Guidelines
Antibiotic resistance is a growing problem. This makes treating pneumococcal pneumonia more complex. The latest guidelines aim to fight the disease effectively while avoiding resistance.
Evolution of Treatment Approaches
Treatment for pneumococcal pneumonia has changed a lot. At first, penicillin was the main treatment. But, as Streptococcus pneumoniae became resistant to penicillin, new guidelines were needed.
Now, doctors often use a combination of antibiotics. This mix usually includes a beta-lactam like ceftriaxone or amoxicillin-clavulanate. Sometimes, a macrolide or fluoroquinolone is added too.
First-Line Antibiotic Therapy
Choosing the right antibiotic depends on several things. These include how severe the disease is, the patient’s health, and local resistance patterns. For mild cases, oral antibiotics like amoxicillin or azithromycin might be used.
Recommended First-Line Antibiotic Therapies:
|
Antibiotic Class |
Examples |
Comments |
|---|---|---|
|
Beta-lactam antibiotics |
Ceftriaxone, Amoxicillin-clavulanate |
Effective against a wide range of S. pneumoniae strains |
|
Macrolides |
Azithromycin, Clarithromycin |
Often used in combination with beta-lactams |
|
Fluoroquinolones |
Levofloxacin, Moxifloxacin |
Reserved for patients with contraindications to other classes |
Treatment Duration and Administration Routes
Antibiotics for pneumococcal pneumonia last from 7 to 14 days. The exact time depends on how severe the disease is and how well the patient responds. At first, patients in the hospital often get antibiotics through an IV. Once they start getting better, they switch to oral antibiotics.
Monitoring Treatment Response
It’s important to watch how the patient is doing. They should start to get better within 48-72 hours of starting antibiotics. If they don’t, it might mean the treatment needs to change.
Regular check-ups with the doctor are key. This helps make sure the treatment is working and addresses any issues that come up.
Severity Assessment and Treatment Stratification
Managing pneumococcal pneumonia starts with a severity assessment. This helps doctors choose the right treatment for each patient. It ensures the best care for those affected.
Pneumonia Severity Index (PSI)
The Pneumonia Severity Index (PSI) is a key tool for doctors. It looks at age, health conditions, and lab results. This system sorts patients by risk, guiding treatment and care.
Key components of the PSI include:
- Demographic characteristics
- Comorbid conditions
- Physical examination findings
- Laboratory and radiographic results
CURB-65 Criteria
The CURB-65 criteria help doctors assess pneumonia severity. It focuses on confusion, uremia, respiratory rate, blood pressure, and age. Each factor gets a point, helping decide treatment.
The CURB-65 criteria are as follows:
- Confusion
- Uremia (elevated blood urea nitrogen)
- Respiratory rate ≥ 30 breaths per minute
- Low blood pressure (systolic
- Age ≥ 65 years
Treatment Protocols Based on Severity
Treatment for pneumococcal pneumonia varies by severity. Mild cases might get oral antibiotics at home. But severe cases need hospital care and IV antibiotics.
Treatment stratification is key for:
- Optimizing antibiotic therapy
- Reducing the risk of complications
- Improving patient outcomes
Using PSI and CURB-65, doctors can tailor treatments. This approach improves care quality for each patient.
Antibiotic Resistance Considerations
Antibiotic resistance is making treating pneumococcal pneumonia harder. The rise of resistant Streptococcus pneumoniae strains is a big problem. We need to understand resistance, find ways to fight it, and look to the future for treatments.
Emerging Resistance Patterns
More cases of penicillin resistance are being seen. This is because of “replacement strains” from overusing certain vaccines. We now have to use different antibiotics to treat this disease.
But it’s not just penicillin that’s a problem. Other antibiotics are also facing resistance. This makes finding effective treatments harder. It’s very important to keep an eye on how resistance is changing.
Strategies to Combat Resistance
We need a strong plan to fight antibiotic resistance. This includes finding new antibiotics, better use of current ones, and tracking resistance. Antibiotic stewardship programs are key in making sure antibiotics are used right.
- Implementing guidelines for antibiotic use
- Monitoring antibiotic consumption
- Educating healthcare providers and patients about antibiotic resistance
Future Directions in Antimicrobial Therapy
The future of fighting infections is bright. We’re working on new antibiotics and other treatments. Bacteriophage therapy is one area showing promise.
Antibiotic Stewardship Programs
Antibiotic stewardship programs are vital in the fight against resistance. They help make sure antibiotics are used wisely. This means fewer unnecessary prescriptions and better treatment for pneumococcal pneumonia.
These programs need everyone’s help. Healthcare providers, policymakers, and patients must work together. Together, we can tackle antibiotic resistance and improve treatment for pneumococcal pneumonia.
Inpatient vs. Outpatient Management
Deciding whether to treat pneumococcal pneumonia in the hospital or at home is important. We look at how sick the patient is, their overall health, and the chance of serious problems. These factors help us decide the best place for treatment.
Criteria for Hospitalization
Patients with very bad pneumococcal pneumonia or those at high risk of serious issues should go to the hospital. Severe pneumonia means they are having trouble breathing, not getting enough oxygen, or their heart is not stable. We also think about sending patients to the hospital if they have other serious health problems or are very young or old.
Guidelines say to hospitalize if:
- They breathe more than 30 times a minute
- They are very distressed while breathing
- They don’t have enough oxygen (PaO2/FiO2 ratio
- The pneumonia is in more than one part of the lung
- They are confused or their mind is not clear
- Their blood pressure is too low (systolic blood pressure
Outpatient Treatment Protocols
For those who don’t need to stay in the hospital, we have plans for treating them at home. Outpatient treatment works for patients with mild to moderate pneumonia who are unlikely to have serious problems.
Home treatment includes:
- Following the recommended antibiotics
- Watching how they feel and how they’re doing
- Seeing a doctor again soon to check on their progress
Monitoring and Follow-up Requirements
Keeping an eye on patients and following up is key for both hospital and home care. For those at home, we want to see them within 48 hours. This is to check how they’re doing and make any needed changes to their treatment.
Transitioning from Hospital to Home Care
When moving a patient from the hospital to their home, we plan carefully. We make sure they’re getting better, their oxygen levels are good, and they can eat normally before sending them home. Discharge criteria include:
- They haven’t had a fever for at least 24 hours
- Their symptoms are getting better
- They can breathe well without extra oxygen
- They can eat normally
A recent study points out, “Moving a patient from the hospital to their home is a key time. It needs careful planning to avoid going back to the hospital and to help them keep getting better.”
“Good planning for leaving the hospital and support after leaving is key for the best results.”
Complications and Management
It’s important to know the complications of pneumococcal pneumonia to manage the disease well. This disease can cause mild to severe problems, mainly in older people and those with health issues.
Common Complications
Some common issues with pneumococcal pneumonia include:
- Respiratory Failure: This happens when the lungs can’t get enough oxygen, often needing a machine to breathe.
- Sepsis: A serious condition where the body attacks its own tissues and organs due to infection.
- Acute Respiratory Distress Syndrome (ARDS): A severe lung issue that stops enough oxygen from getting to the blood.
Management of Complications
Managing complications well is key to better patient results. We use a variety of methods, including:
- Early Recognition: Spotting complications early helps us act fast.
- Supportive Care: Giving care like oxygen and breathing machines when needed.
- Antimicrobial Therapy: Using the right medicines to fight the infection.
Long-term Outcomes and Prognosis
The long-term results for patients with pneumococcal pneumonia can differ a lot. The severity of the problem, the patient’s health, and how quickly and well they’re treated all play a role. We help patients and their families with care and support all the way through recovery.
Recovery and Rehabilitation
The journey to get better from pneumococcal pneumonia includes rest, good nutrition, and pulmonary rehab. It’s key to know how long it takes to get better, the role of rehab, and the value of eating right.
Expected Recovery Timeline
How long it takes to get better from pneumococcal pneumonia varies. Some people start feeling better in a week, while others may take a month or more. It’s important to listen to your doctor’s advice to recover well.
Pulmonary Rehabilitation
Pulmonary rehab is a big help in getting better. It helps patients get their lung function and strength back. By doing pulmonary rehab, patients can improve their recovery a lot.
Nutritional Support
Good nutrition is key to getting better. It gives the body what it needs to heal and get strong. Eating a balanced diet with proteins, vitamins, and minerals helps the immune system. Getting nutritional advice from a doctor can help make a diet plan that’s right for you.
Follow-up Care and Monitoring
Regular check-ups are important to see how you’re doing and catch any problems early. Going to your doctor’s appointments helps make sure you’re on the right track to getting better. Going to all your follow-up appointments is important for the best results.
Conclusion
Pneumococcal pneumonia is a serious infection caused by Streptococcus pneumoniae. It needs quick and effective treatment. We’ve looked at its causes, symptoms, diagnosis, and treatment options in this guide.
Knowing how to treat pneumococcal pneumonia is key. Healthcare providers can start the right antibiotic therapy early. This helps improve patient outcomes.
Treating pneumococcal pneumonia requires a detailed plan. This includes assessing how severe it is and choosing the right treatment. Both inpatient and outpatient care are important. Knowing about possible complications helps in giving the best care.
With antibiotic resistance growing, fighting it is critical. Healthcare providers need to stay up-to-date with the latest treatment guidelines. This way, they can give the best care to patients with pneumococcal pneumonia.
Managing pneumococcal pneumonia well needs a team effort. From prevention to treatment and rehabilitation, we must work together. This way, we can lessen the disease’s impact and improve health outcomes for those affected.
FAQ
What is pneumococcal pneumonia?
Pneumococcal pneumonia is caused by the bacterium Streptococcus pneumoniae. It can lead to severe respiratory illness.
What are the symptoms of pneumococcal pneumonia?
Symptoms range from mild to severe. They include cough, fever, and difficulty breathing. Severe symptoms include high fever, chills, and chest pain.
How is pneumococcal pneumonia diagnosed?
Diagnosis involves a physical exam, lab tests, and imaging studies. This includes microbiological confirmation methods.
What is the treatment for pneumococcal pneumonia?
Treatment involves antibiotics. The type and duration depend on the disease’s severity and patient factors.
What are the risk factors for developing pneumococcal pneumonia?
Risk factors include age, underlying health conditions, and lifestyle factors. Elderly and young children are at higher risk.
How is the severity of pneumococcal pneumonia assessed?
Severity is assessed using tools like the Pneumonia Severity Index (PSI) and CURB-65 criteria. These guide treatment decisions.
What are the possible complications of pneumococcal pneumonia?
Complications include respiratory failure, sepsis, and long-term lung damage. These can be serious.
How can pneumococcal pneumonia be prevented?
Prevention includes vaccination against Streptococcus pneumoniae. It’s key for high-risk populations. Healthy lifestyle choices also help.
What is the role of antibiotic stewardship in treating pneumococcal pneumonia?
Antibiotic stewardship programs aim to improve antibiotic use. They reduce resistance and enhance treatment outcomes for pneumococcal pneumonia.
What is the expected recovery timeline for pneumococcal pneumonia?
Recovery times vary based on disease severity and patient factors. Symptoms usually improve gradually over weeks.
What is pneumococcal disease?
Pneumococcal disease includes infections caused by Streptococcus pneumoniae. This includes pneumonia, meningitis, and otitis media.
What is Streptococcus pneumoniae?
Streptococcus pneumoniae is a bacterium. It can cause various infections, including pneumococcal pneumonia.
References
National Center for Biotechnology Information. Evidence-Based Medical Guidance. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7112285/


































