Learn the warning signs of Myelogenous Leukemia. From sudden AML symptoms like petechiae to the slow progression of CML and splenomegaly.
Send us all your questions or requests, and our expert team will assist you.
Myelogenous Leukemia: Conditions and Indications
Conditions and indications in myelogenous leukemia describe the clinical situations in which advanced therapeutic strategies, including stem cell–based approaches, may be considered as part of disease management. Because myelogenous leukemia encompasses biologically diverse diseases with variable progression patterns, indications are not uniform and depend on disease type, response to initial therapy, and overall bone marrow function. The goal of identifying appropriate indications is to determine when restoration of healthy blood formation becomes a central therapeutic priority.
In the context of stem cell treatment, myelogenous leukemia itself is evaluated as the underlying condition that may warrant replacement or reconstitution of diseased bone marrow under specific circumstances. This decision is based on careful clinical assessment rather than on diagnosis alone.
Different clinical forms of myelogenous leukemia create different therapeutic considerations.
Acute myelogenous leukemia is characterized by aggressive disease behavior and rapid bone marrow failure. In this setting, abnormal myeloid cells quickly dominate the marrow, leading to severe anemia, infection risk, and bleeding tendency.
Conditions commonly associated with acute myelogenous leukemia include
• Rapidly rising blast cell counts
• Severe suppression of normal blood cell production
• High risk of life-threatening complications
Because of this aggressive profile, advanced treatment strategies may be considered when conventional therapies alone are insufficient to achieve durable disease control.
Chronic myelogenous leukemia typically progresses more slowly and may remain stable for extended periods. However, disease behavior can change over time, particularly if progression accelerates or treatment response diminishes.
Clinical conditions influencing advanced treatment consideration include
• Disease progression despite standard therapy
• Transition to more aggressive disease phases
• Increasing bone marrow dysfunction
In these situations, restoring normal marrow function becomes an important therapeutic objective.

Disease progression plays a central role in determining indications.
When myelogenous leukemia does not respond adequately to standard treatment or shows signs of ongoing progression, alternative strategies may be evaluated. Persistent abnormal cell growth can lead to cumulative marrow damage and declining blood counts.
Indicators of inadequate disease control may include
• Worsening blood count abnormalities
• Increasing marrow involvement
• Recurrent disease activity after initial response
These findings suggest the need for reassessment of long-term treatment strategy.

Bone marrow health is a key determinant in advanced therapy planning.
When the bone marrow’s ability to produce healthy blood cells is significantly impaired, supportive treatments alone may not be sufficient. In such cases, approaches aimed at reestablishing normal hematopoiesis may be considered.
Clinical features supporting this indication include
• Chronic dependence on transfusion support
• Recurrent infections due to immune suppression
• Persistent bleeding risk related to low platelet production
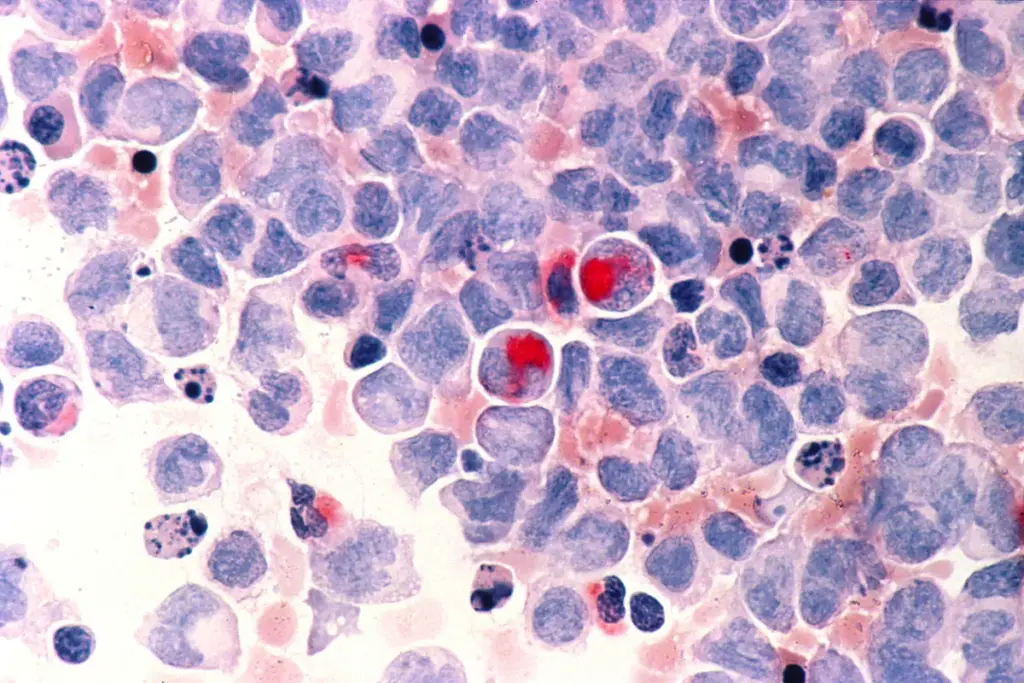
Not all cases of myelogenous leukemia behave the same way.
Certain biological and genetic features are associated with more aggressive disease behavior and reduced responsiveness to conventional treatment. When these features are present, clinicians may consider advanced treatment pathways earlier in the disease course.
Risk stratification helps identify individuals who may benefit from more definitive marrow-directed strategies.
Beyond disease characteristics, patient factors are also important.
Advanced treatments are considered only when a patient’s overall condition allows for intensive therapy. Factors such as organ function, age-related physiological reserve, and ability to tolerate immune suppression are carefully evaluated.
Indications therefore reflect a balance between disease severity and patient suitability.
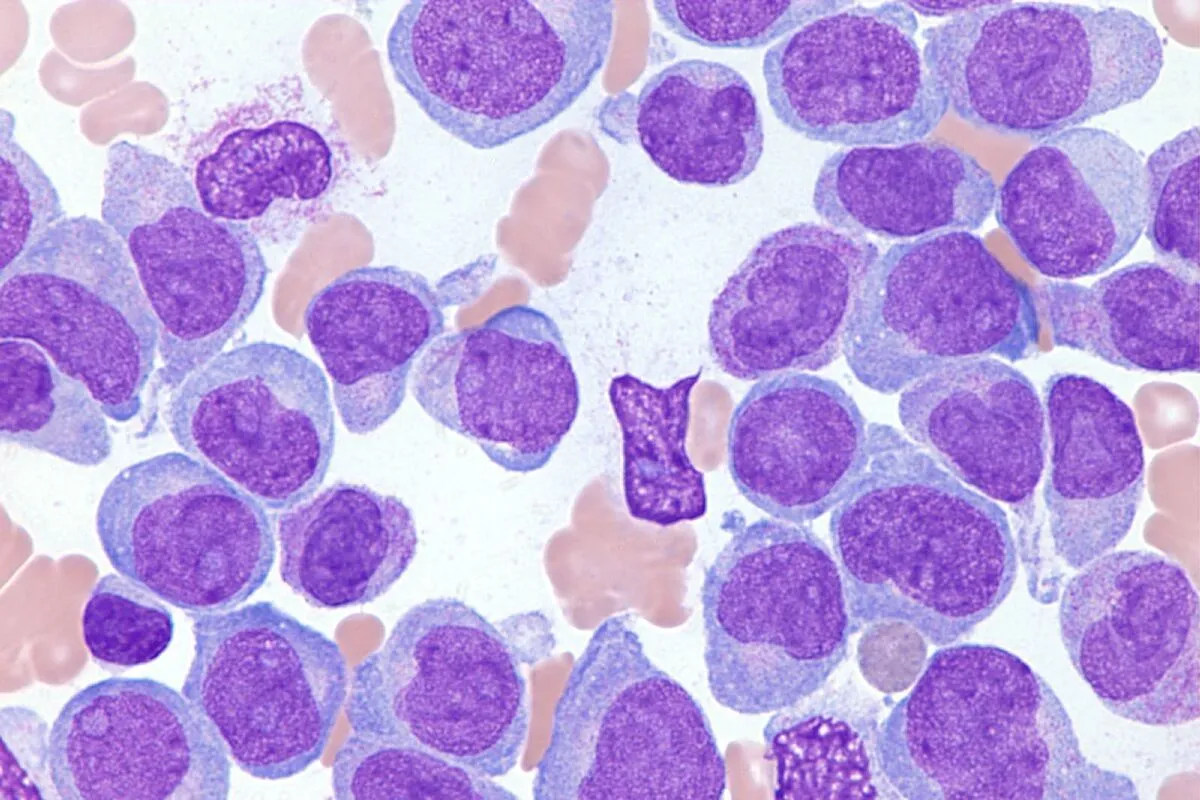
Timing is a critical element in determining indications.
In some cases, earlier intervention may offer better long-term disease control, while in others, delaying advanced treatment until clear progression occurs may be more appropriate. This decision is individualized and based on ongoing assessment rather than fixed timelines.
Identifying appropriate conditions and indications ensures that advanced treatments, including stem cell–based strategies, are applied when potential benefits outweigh risks. Careful selection helps avoid unnecessary intervention while preserving the option for definitive treatment when disease behavior warrants it.
By aligning indications with disease biology and patient condition, clinicians aim to support long-term disease control and restoration of healthy blood cell production.

Send us all your questions or requests, and our expert team will assist you.
No, many patients are managed successfully with standard therapies.
It is considered when disease progression or marrow failure becomes significant.
Yes, aggressive disease behavior often leads to consideration of intensive approaches.
No, but progression can occur and requires close monitoring.
Yes, overall health and treatment tolerance are essential considerations.

 Myelogenous Leukemia
Myelogenous Leukemia Myelogenous Leukemia
Myelogenous Leukemia Myelogenous Leukemia
Myelogenous Leukemia Myelogenous Leukemia
Myelogenous Leukemia Myelogenous Leukemia
Myelogenous Leukemia Myelogenous Leukemia
Myelogenous Leukemia
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)