How is Myelogenous Leukemia diagnosed? Learn about the essential tests from bone marrow biopsy and blast counts to genetic profiling for AML and CML.
Send us all your questions or requests, and our expert team will assist you.
Myelogenous Leukemia: Diagnosis and Evaluation
Diagnosis and evaluation of myelogenous leukemia aim to confirm the presence of malignant myeloid cells, define the specific disease subtype, and assess the extent of bone marrow involvement in order to guide treatment decisions, including consideration of stem cell–based therapies. Because myelogenous leukemia directly affects the bone marrow’s ability to produce healthy blood cells, evaluation is comprehensive and integrates laboratory findings, marrow assessment, and biological risk profiling.
In the context of stem cell treatment, diagnosis and evaluation are especially important because they determine whether the disease burden, marrow function, and biological characteristics justify a treatment approach focused on replacing or reconstituting the diseased bone marrow. Accurate evaluation ensures that advanced therapies are applied appropriately and at the right stage of the disease.
Evaluation typically begins with routine laboratory testing that raises suspicion for myelogenous leukemia.
A complete blood count often reveals characteristic changes that prompt further investigation.
Common findings may include
• Elevated or abnormally low white blood cell counts
• Reduced red blood cell levels causing anemia
• Low platelet counts increasing bleeding risk
These abnormalities reflect disruption of normal bone marrow function by malignant myeloid cells.
Microscopic analysis of blood cells provides important diagnostic clues.
Examination of a blood smear allows assessment of cell size, shape, and maturity. In acute myelogenous leukemia, immature blast cells are often prominent, while chronic myelogenous leukemia shows more mature appearing myeloid cells in excess.
This evaluation helps
• Differentiate acute from chronic disease
• Identify abnormal myeloid patterns
• Support further diagnostic testing
Bone marrow assessment is central to diagnosis and evaluation.
Sampling the bone marrow provides direct insight into disease involvement and severity. It reveals the proportion of abnormal myeloid cells and the degree to which normal blood-forming cells have been replaced.
Bone marrow examination is used to
• Confirm the diagnosis
• Determine disease burden
• Assess marrow reserve and recovery potential
This information is essential when evaluating eligibility for stem cell–based treatment.
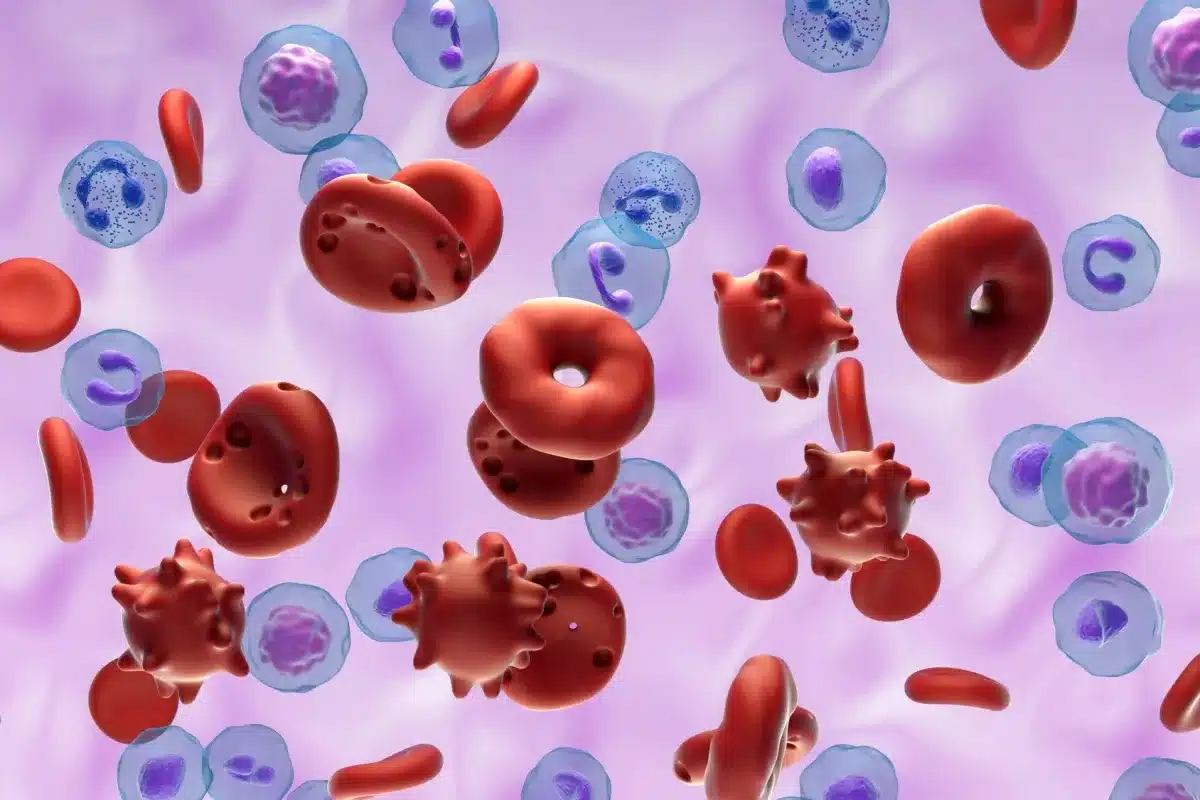
Identifying the exact type of abnormal cells is a critical step.
Immunophenotyping uses cell surface markers to confirm that malignant cells originate from the myeloid lineage rather than lymphoid cells. This distinction ensures accurate classification and avoids misdiagnosis.
Precise lineage identification supports
• Correct disease classification
• Selection of appropriate treatment pathways
• Risk assessment for disease progression
Modern evaluation includes detailed analysis of genetic features.
Genetic testing identifies chromosomal and molecular abnormalities that influence disease behavior, treatment response, and long-term outlook. These features play a major role in determining whether stem cell treatment is considered.
Genetic evaluation helps
• Stratify disease risk
• Predict likelihood of treatment resistance
• Guide timing of advanced therapy consideration
Disease phase is particularly important in chronic myelogenous leukemia.
Chronic myelogenous leukemia may progress through different phases, each with distinct clinical implications. Evaluation focuses on identifying whether the disease remains stable or shows signs of acceleration.
Understanding disease phase supports
• Appropriate treatment intensity
• Early identification of progression
• Long-term planning for marrow-directed therapies
Myelogenous leukemia may affect organs beyond the bone marrow.
Clinical examination and imaging may be used to evaluate enlargement of the spleen or liver and to assess overall disease distribution. These findings contribute to staging and risk assessment.

Evaluation extends beyond disease characteristics alone.
Because stem cell treatment involves significant immune and marrow impact, patient-related factors are carefully assessed. These include overall health status, organ function, and ability to tolerate intensive therapy.
This assessment ensures that potential benefits outweigh risks.

Diagnosis and evaluation culminate in an integrated disease profile.
By combining laboratory results, marrow findings, genetic features, and patient condition, clinicians develop a complete understanding of disease behavior. This integrated profile guides decisions regarding conventional therapy, timing of intervention, and consideration of stem cell–based treatment strategies.
Accurate and comprehensive evaluation is essential for safe and effective management of myelogenous leukemia. It ensures that treatment decisions are evidence-based, individualized, and aligned with both disease biology and patient readiness.
In the context of stem cell treatment, thorough evaluation protects patients from unnecessary risk while preserving the option for definitive marrow restoration when clinically appropriate.

Send us all your questions or requests, and our expert team will assist you.
Through blood tests, bone marrow examination, and cell analysis.
It shows the extent of disease and marrow function.
Yes, they strongly influence risk assessment and therapy planning.
Yes, each form requires tailored assessment.
Yes, it is essential for determining suitability and timing.

 Myelogenous Leukemia
Myelogenous Leukemia Myelogenous Leukemia
Myelogenous Leukemia Myelogenous Leukemia
Myelogenous Leukemia Myelogenous Leukemia
Myelogenous Leukemia Myelogenous Leukemia
Myelogenous Leukemia
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)