Pulmonology focuses on diagnosing and treating lung and airway conditions such as asthma, COPD, and pneumonia, as well as overall respiratory health.
Send us all your questions or requests, and our expert team will assist you.
Chronic bronchitis is a serious, ongoing change in the structure of the lower airways and is part of Chronic Obstructive Pulmonary Disease (COPD). It is not just about symptoms, but about specific changes in the bronchial tubes. The disease mainly affects the bronchi, which carry air from the windpipe to the parts of the lungs where gas exchange happens. Normally, these airways are lined with tiny hairs and mucus-producing cells that help trap and remove dust and germs. In chronic bronchitis, this defense system breaks down.
The main problem is long-lasting inflammation in the lining of the bronchi, usually due to breathing in harmful substances like tobacco smoke over many years. This leads to changes in the airway walls. The mucus glands become larger and more numerous, occupying a greater proportion of the airway wall (as measured by the Reid Index). At the same time, the tiny hairs that help move mucus are damaged or lost, so mucus builds up. The airway walls become swollen and scarred, narrowing the airways permanently. This narrowing, along with mucus blockages, makes it much harder to exhale, which causes the main symptoms of the disease. At Liv Hospital, we focus on understanding these changes to guide our treatments and address the main causes of blockage and inflammation.
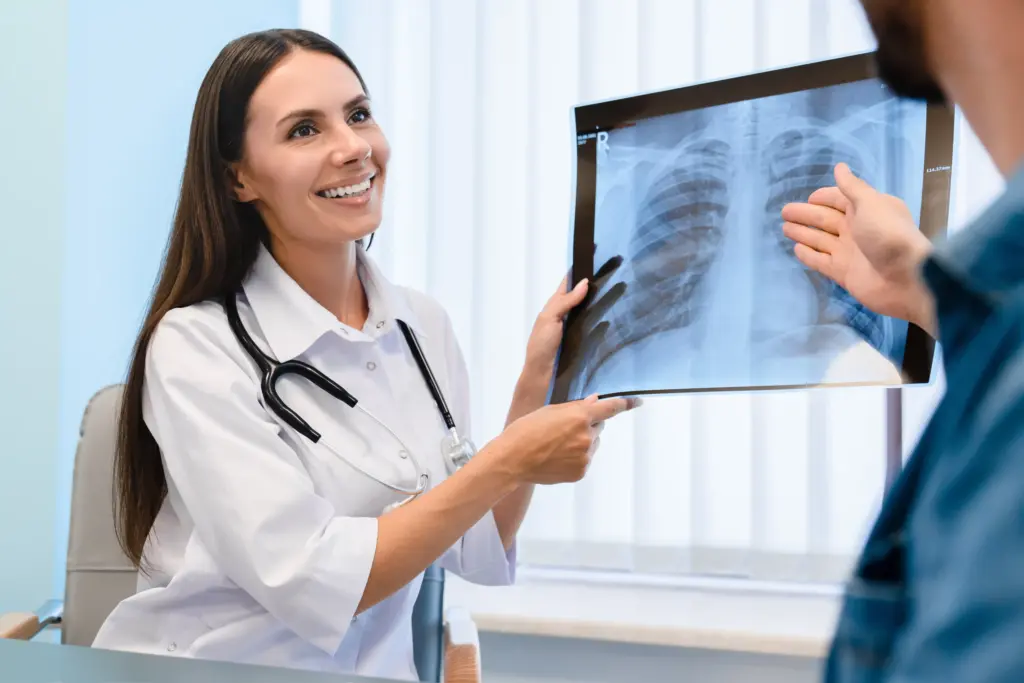
Doctors define chronic bronchitis by a clear pattern: a cough that brings up mucus and lasts for at least three months in each of two years in a row, after ruling out other causes like bronchiectasis, tuberculosis, or lung cancer. This definition is based on how the disease behaves over time, showing that it is long-lasting and tends to come back. It helps separate chronic bronchitis from acute bronchitis, which is a short-term infection, and from a smoker’s cough, which can go away if the person stops smoking. Having this diagnosis means the disease is likely to get worse without treatment. The cough is the body’s way of trying to clear out extra mucus that the damaged airway hairs can’t move. Over time, this cough becomes part of daily life, often worse in the morning as mucus builds up overnight. The definition also includes “acute exacerbations,” which are times when symptoms suddenly get worse, often due to infection or pollution, and these episodes can cause lasting drops in lung function.
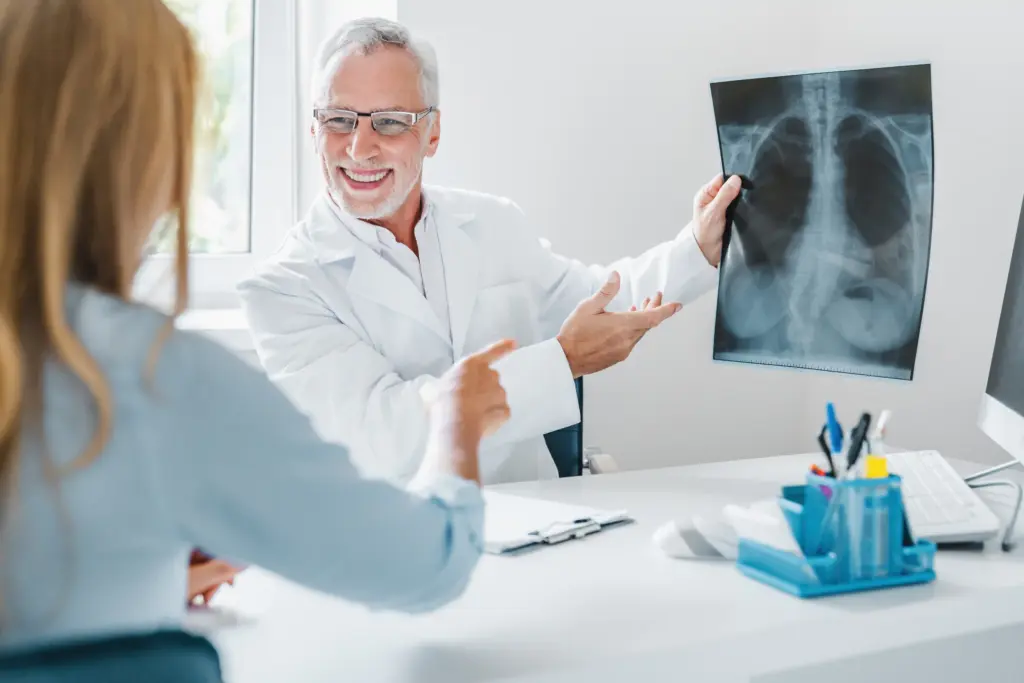
Traditionally, doctors have described people with chronic bronchitis as having the “Blue Bloater” type, while those with emphysema are called “Pink Puffers.” Most people actually have a mix of both, but the Blue Bloater description helps explain the specific problems seen in severe chronic bronchitis.
Chronic bronchitis usually does not occur alone. It is part of the COPD group, along with emphysema, which is marked by the destruction of the air sacs in the lungs and their permanent enlargement. Chronic bronchitis blocks the airways with mucus and inflammation, while emphysema causes the lungs to lose their stretchiness and surface area. Most smokers with COPD have both problems, but one may be more severe. Knowing which type is more prominent helps guide treatment. For example, people with more emphysema may benefit from lung volume reduction, while those with more mucus may do better with certain medications that thin mucus. Chronic bronchitis can also overlap with asthma, called Asthma-COPD Overlap (ACO), which involves some reversible airway blockage and a different type of inflammation. This overlap needs a different treatment plan, often starting inhaled steroids sooner.
Chronic bronchitis is a major health problem around the world, affecting millions of people. It is most common where tobacco smoking is widespread, since smoking is the main cause. In lower-income countries, indoor air pollution from burning wood, animal dung, or crop waste for cooking and heating is also a major cause, especially for women and children. Jobs that expose people to dust, chemicals, or fumes add to the risk. The disease becomes more common with age and has been more frequent in men, but as more women smoke, the gap is closing. Chronic bronchitis leads to a lot of lost healthy years because it limits activity and causes frequent hospital stays. It also affects poorer communities more, due to higher smoking rates, more job exposures, and worse living conditions.
On a molecular level, chronic bronchitis develops because there is an imbalance between harmful oxidants and the body’s antioxidants. Cigarette smoke contains huge amounts of free radicals and other oxidants up to a million billion per puff. These substances damage the fats, proteins, and DNA in lung cells and deplete the lung’s natural antioxidants, such as glutathione. This stress triggers signals inside cells that turn on genes, causing inflammation, bringing more immune cells into the airways. This ongoing damage not only causes inflammation but also makes steroid treatments less effective, so chronic bronchitis is harder to treat with steroids than asthma. Understanding these processes is important for finding new treatments that target this kind of damage.
Although chronic bronchitis is usually defined by changes in the larger airways, a lot of damage also happens in the small airways, called bronchioles, which are less than 2mm wide. In chronic bronchitis, these small airways become inflamed, scarred, and blocked with mucus. Because there are so many of these small airways, a lot of disease can build up here without showing up on standard lung tests until things are quite advanced. This small airway disease is a big reason for the increased resistance and air trapping seen in COPD. New imaging and testing methods are helping doctors find these changes earlier, which may allow for earlier treatment before permanent damage occurs.

Send us all your questions or requests, and our expert team will assist you.
The constant irritation from smoke or pollutants causes the mucus-producing glands in the airways to grow larger and multiply, producing way more mucus than usual to try to protect the lining.
While usually caused by the environment, a genetic condition called Alpha-1 Antitrypsin Deficiency can make people develop severe bronchitis and emphysema at a young age, even if they never smoke.
Yes, long-term exposure to second-hand smoke, severe air pollution, chemical fumes at work, or dust from mining/agriculture can cause the disease in non-smokers.
Yes, the low oxygen levels can strain the heart, leading to heart failure, cause muscle wasting and weakness, and increase the risk of osteoporosis and depression.
The scarring and structural changes are essentially permanent, but quitting stops the active inflammation, allowing some healing, reducing mucus, and significantly slowing further damage.


Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)