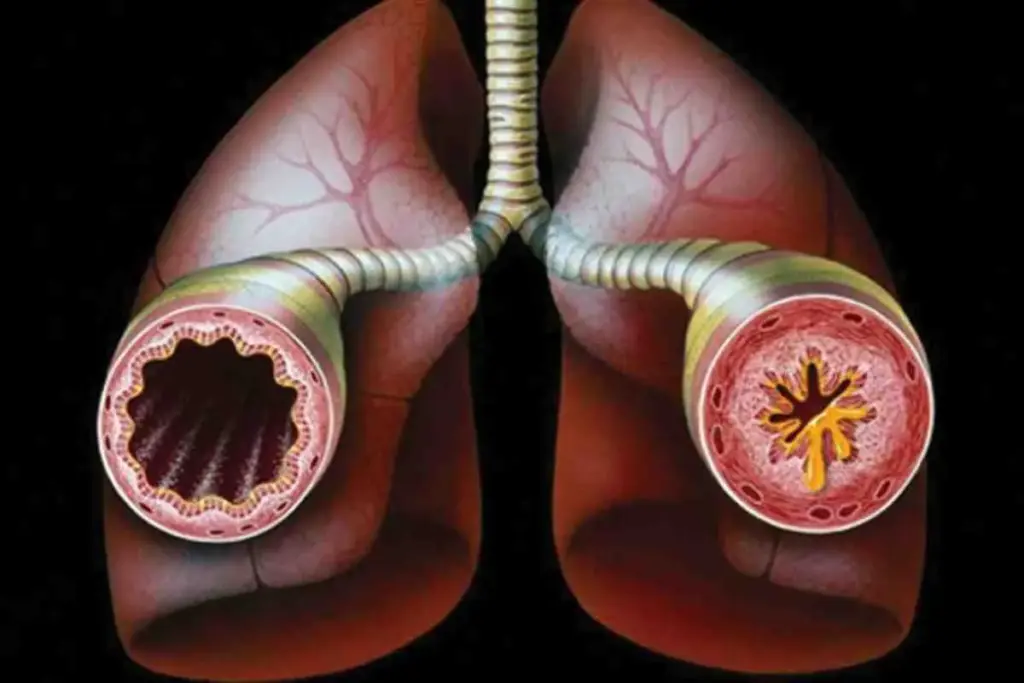
Have you ever gotten a diagnosis of bronchial wall thickening after a chest scan? You might wonder what it means for your health. This condition, also known as peribronchial thickening or cuffing, shows airway inflammation.
We’ll talk about what makes thickened bronchial walls happen and when you should worry. Bronchial wall thickening can be due to long-term inflammation like asthma and COPD, or infections. Knowing why it happens is key for early diagnosis and treatment.
Key Takeaways
- Bronchial wall thickening is a sign of airway inflammation seen on scans.
- Long-term inflammation from asthma and COPD can cause thickened bronchial walls.
- Infections are also a big reason for bronchial wall thickening.
- Understanding the causes is vital for early diagnosis and treatment.
- Chest scans like CT scans can spot bronchial wall thickening.
Understanding Bronchial Wall Thickening
To understand bronchial wall thickening, we need to know what it is. It’s when the walls of the bronchi, the airways leading to the lungs, get thicker. This can be a sign of many things, from mild inflammation to serious diseases.
What Is Bronchial Wall Thickening?
Bronchial wall thickening means the walls of the bronchi get thicker. Doctors can see this on chest X-rays and CT scans. It can happen due to inflammation, infection, or other diseases. Some cases might have just a little thickening, while others can be more severe.
Types of Bronchial Wall Thickening
There are different types of bronchial wall thickening, depending on the cause and how bad it is. Here are a few:
- Mild peribronchial thickening, often seen in mild inflammation or infection.
- Bilateral peribronchial thickening, showing a condition affecting both lungs.
- Perihilar bronchial wall thickening, where thickening is more around the lung’s hilar regions.
The type and how severe it is can help doctors understand the problem better. It helps them decide what tests and treatments are needed.
How Bronchial Wall Thickening Is Detected
Doctors use imaging studies to find bronchial wall thickening. Chest X-rays might show signs, but CT scans are better. CT scans are great for seeing how bad the thickening is and if there are other problems like bronchiectasis or air trapping.
Common Causes of Bronchial Wall Thickening and Associated Risks
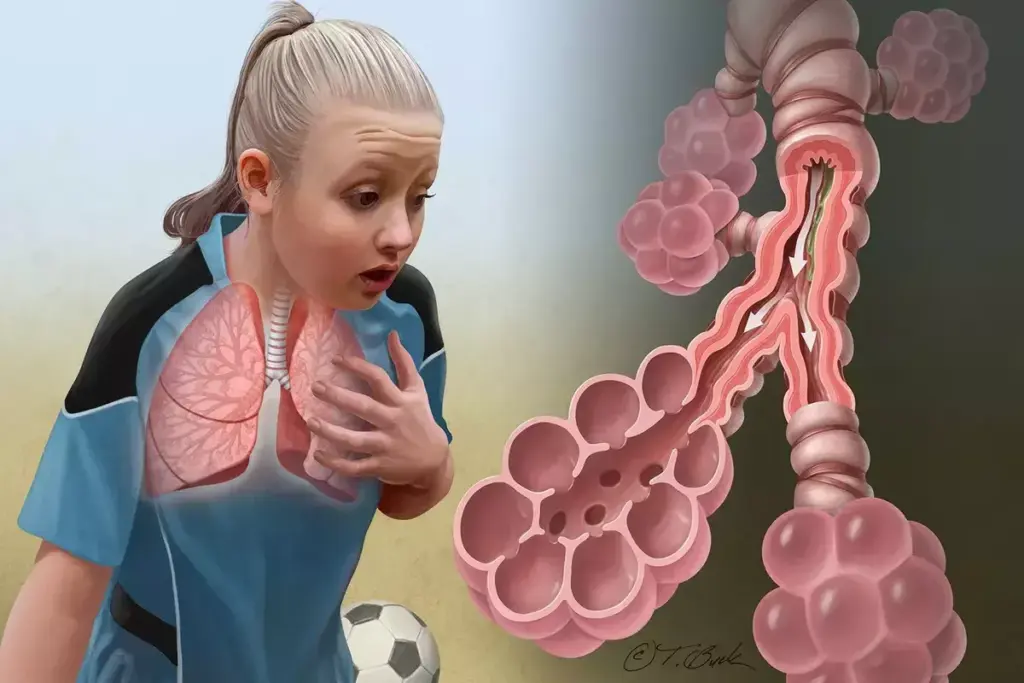
Bronchial wall thickening can be caused by many factors, like inflammation and infections. Knowing these causes is key for proper diagnosis and treatment.
Inflammatory Conditions
Chronic inflammation is a big reason for bronchial wall thickening. Conditions like asthma and chronic obstructive pulmonary disease (COPD) cause long-term inflammation. This makes the bronchial walls thicken, narrowing the airways and making symptoms worse.
Asthma, in particular, changes the bronchial walls a lot. The inflammation from asthma can lead to:
- Increased mucus production
- Airway hyperresponsiveness
- Remodeling of the airway walls
These changes make it harder for air to move through the bronchial walls.
Infectious Causes
Infections also play a big role in bronchial wall thickening. Respiratory infections, like pneumonia and bronchitis, can cause inflammation and damage. This damage can sometimes lead to long-term thickening of the bronchial walls.
| Infectious Agent | Common Symptoms | Potential Complications |
| Bacteria (e.g., Streptococcus pneumoniae) | Cough, fever, difficulty breathing | Pneumonia, sepsis |
| Viruses (e.g., Influenza virus) | Cough, sore throat, fever | Bronchitis, pneumonia |
Other Medical Conditions
Other medical conditions can also cause bronchial wall thickening. For example, gastroesophageal reflux disease (GERD) can cause stomach acid to flow up into the lungs. This can irritate and inflame the bronchial walls.
In conclusion, bronchial wall thickening is a complex issue that needs a detailed approach for diagnosis and treatment. By understanding the different causes, healthcare providers can create effective treatment plans.
Conclusion: When to Seek Medical Attention
Knowing what causes bronchial wall thickening is key to taking the right steps. Mild thickening might show signs of health issues that need a doctor’s check-up.
Signs like a long-lasting cough, lots of mucus, or coughing up blood mean you should see a doctor. Thickening near the lungs, often due to infections or inflammation, also needs quick attention.
Keep an eye on your health and get medical help if you notice unusual breathing symptoms. Learning about bronchial wall thickening can help you stay healthy.
FAQ
What is bronchial wall thickening?
Bronchial wall thickening is the enlargement of the airway walls due to inflammation, infection, or chronic irritation.
What are the types of bronchial wall thickening?
Types include diffuse, segmental, or focal thickening, depending on the extent and location in the lungs.
How is bronchial wall thickening detected?
It is detected using imaging tests like high-resolution CT scans or chest X-rays.
What causes bronchial wall thickening?
Causes include chronic bronchitis, asthma, infections, smoking, and environmental irritants.
Is bronchial wall thickening a sign of a serious condition?
It can indicate underlying chronic lung disease, but severity depends on the cause and progression.
Can bronchial wall thickening be treated?
Treatment focuses on addressing the underlying cause, reducing inflammation, and managing symptoms.
What are the risks associated with bronchial wall thickening?
Risks include recurrent infections, reduced lung function, and progression to chronic respiratory conditions.
How can I prevent bronchial wall thickening?
Avoid smoking, manage asthma or infections promptly, minimize exposure to irritants, and maintain lung health.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pubmed.ncbi.nlm.nih.gov/24335668/


































